Spina bifida
Overview
Spina bifida is a condition that occurs when the spine and spinal cord don't form properly. It's a type of neural tube defect. The neural tube is the structure in a developing embryo that later becomes the baby's brain and spinal cord and the tissues that enclose them.
Typically, the neural tube forms early in pregnancy and closes by the 28th day after conception. In babies with spina bifida, a portion of the neural tube doesn't close all the way. This affects the spinal cord and bones of the spine.
Spina bifida can range from being mild to causing serious disabilities. Symptoms depend on where on the spine the opening is located and how big it is. Symptoms also depend on whether the spinal cord and nerves are involved. When necessary, early treatment for spina bifida involves surgery. However, surgery doesn't always completely restore lost function.
Types
Spina bifida occurs in different types: spina bifida occulta, myelomeningocele (my-uh-lo-muh-NING-go-seel) or the very rare type, meningocele (muh-NING-go-seel).
Spina bifida occulta
Occulta means hidden. Spina bifida occulta is the mildest and most common type. This type of spina bifida results in a small separation or gap in one or more of the bones of the spine, called vertebrae. Many people who have spina bifida occulta don't know they have it. It may be found during an imaging test such as an X-ray that is done for another reason.
Myelomeningocele
Myelomeningocele is the most serious type. It also is known as open spina bifida. The spinal canal is open along several vertebrae in the lower or middle back. Part of the spinal cord, including the spinal cord's protective covering and spinal nerves, push through this opening at birth, forming a sac on the baby's back. Tissues and nerves usually are exposed. This makes the baby prone to dangerous infections. This type also may cause loss of movement in the legs, and bladder and bowel dysfunction.
Meningocele
This is a rare type of spina bifida. In this type, a sac of spinal fluid bulges through an opening in the spine. No nerves are affected and the spinal cord isn't in the fluid sac. Babies with meningocele may have some minor trouble with functioning, including with the bladder and bowels.
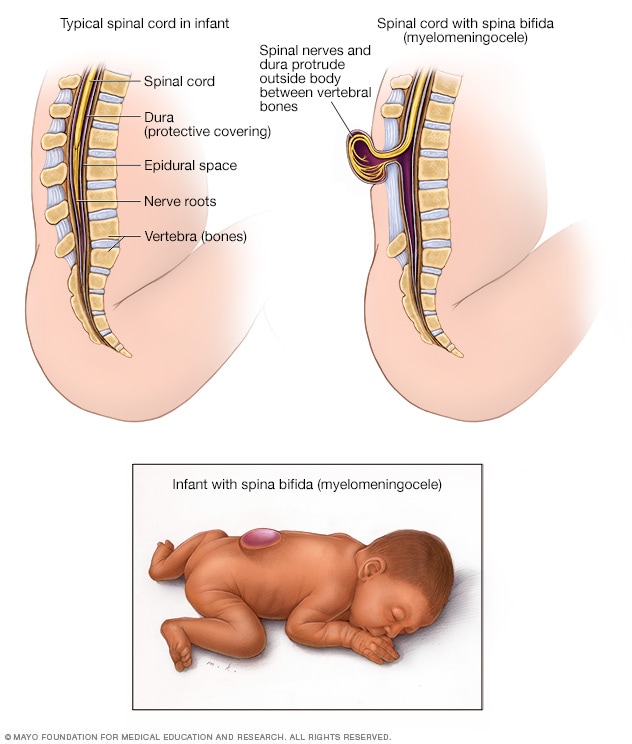
Myelomeningocele is the most serious type of spina bifida. The spinal cord's protective covering and the spinal nerves protrude at birth, forming a sac on the baby's back. The exposed nervous system may become infected, so prompt surgery is needed after birth.
Symptoms
Symptoms of spina bifida vary by type and from one person to another.
- Spina bifida occulta. Typically, there aren't any symptoms of spina bifida occulta because the spinal nerves aren't involved. But you can sometimes see symptoms on the newborn's skin above the small gap in the spine. You might see a tuft of hair, a small dimple or a birthmark. Sometimes, these skin marks can be symptoms of a spinal cord issue that can be found with MRI or a spinal ultrasound in a newborn.
- Meningocele. This type may affect bladder and bowel function.
- Myelomeningocele. In this most serious type of spina bifida, the spinal canal remains open along several vertebrae in the lower or middle back. The membranes and part of the spinal cord or nerves protrude at birth, forming a sac. Tissues and nerves usually are exposed, though sometimes skin covers the sac. Babies with this type of spina bifida may have trouble with bladder and bowel function. They also may experience weakness or lack of movement in the legs. Babies may have a buildup of fluid in the brain called hydrocephalus that can put pressure on brain tissue.
When to see a doctor
Typically, myelomeningocele is diagnosed before or right after birth, when medical care is available. Children diagnosed with this condition should be followed by a specialized team of healthcare professionals throughout their lives. Families can be educated on the different complications to watch for.
Children with spina bifida occulta typically don't have symptoms or complications. In these children, usually only routine pediatric care is needed.
Causes
The cause of spina bifida is not known. It's thought that a combination of genetic, nutritional and environmental risk factors causes the condition. This includes having a family history of neural tube defects and getting too little folate, also known as vitamin B-9, during pregnancy.
Risk factors
Spina bifida is more common among Hispanic people and white people. Also, female babies are affected more often than male babies. Although healthcare professionals and researchers don't know why spina bifida occurs, they have identified some risk factors:
- Too little folate in the pregnant person's body. Folate, the natural form of vitamin B-9, is important to the development of a healthy baby. Folic acid is the synthetic form that's found in supplements and fortified foods. If folate levels are too low, it's known as a deficiency. Folate deficiency increases the risk of spina bifida and other conditions that affect the neural tube.
-
Family history of neural tube defects. Having one child with a condition that affects the neural tube slightly increases the chance of having another baby with the same condition. The risk increases even more if two previous children have been affected by the condition.
Also, being born with a neural tube defect increases the chance of giving birth to a child with spina bifida. However, most babies with spina bifida are born to parents with no known family history of the condition.
- Some medicines. Taking anti-seizure medicines such as valproic acid during pregnancy increases the risk of having a baby with spina bifida. This might happen because the medicines interfere with the body's ability to use folate and folic acid.
- Diabetes. Having diabetes that is not well controlled before becoming pregnant increases the risk of having a baby with spina bifida.
- Obesity. Obesity at the time of pregnancy also is associated with an increased risk of spina bifida.
- Increased body temperature. Some evidence suggests that increased body temperature in the early weeks of pregnancy may increase the risk of spina bifida. A high core body temperature can be caused by a fever or by using a sauna or hot tub.
If you have known risk factors for spina bifida, talk with your healthcare professional. You may need a larger dose or prescription dose of folic acid, even before a pregnancy begins.
Also tell your healthcare professional about all of the medicines you take. If you plan ahead, some medicines can be adjusted to lower the potential risk of spina bifida.
Complications
Spina bifida may cause minimal symptoms or it can lead to more-serious physical conditions. Symptoms are affected by:
- The size and location of the opening in the spine.
- Whether skin covers the affected area.
- Which spinal nerves come out of the affected area of the spinal cord.
A number of complications may affect children with spina bifida. But not all children get all of these complications. Many complications can be treated.
- Walking and mobility problems. The nerves that control the leg muscles don't work properly below the area of the spinal cord that is affected. This can cause muscle weakness of the legs. Sometimes it can cause loss of movement, known as paralysis. Whether a child can walk depends on the location of the spine that's affected and the size of the opening in the neural tube. Ability to walk also depends on the care received before and after birth.
- Orthopedic complications. Children with myelomeningocele can have several complications in the legs and spine because of weak muscles. The complications depend on the location of the spine that's affected. Possible orthopedic issues may include:
- Curved spine, known as scoliosis.
- Changes that aren't typical, such as an inward-facing foot, known as clubfoot.
- Dislocation of the hip.
- Bone and joint conditions.
- Shortened, tight muscles, known as muscle contractures.
- Bowel and bladder symptoms. Nerves that supply the bladder and bowel usually don't work properly in children with myelomeningocele. As a result, they can't control their bowel or bladder. This is because the nerves that supply the bowel and bladder come from the lowest level of the spinal cord.
- Buildup of fluid in the brain, known as hydrocephalus. Babies born with myelomeningocele commonly have a buildup of fluid in the brain. This condition is known as hydrocephalus.
- Shunt malfunction. Shunts placed in the brain to treat hydrocephalus can stop working or become infected. Warning signs may vary. Some of the warning symptoms of a shunt that isn't working include:
- Headaches.
- Vomiting.
- Sleepiness.
- Irritability.
- Swelling or redness along the shunt.
- Confusion.
- Changes in the eyes, such as a fixed downward gaze.
- Trouble feeding.
- Seizures.
- Chiari malformation type 2. Chiari malformation (kee-AH-ree mal-for-MAY-shun) type 2 is common in children who have myelomeningocele. The brainstem is the lowest part of the brain above the spinal cord. In Chiari malformation type 2, the brainstem becomes longer and is lower than usual in the spinal canal or area of the neck. This can cause arm weakness and trouble with breathing and swallowing. Rarely, this condition can cause compression on this area of the brain. Surgery is needed to relieve the pressure.
- Infection in the tissues surrounding the brain, known as meningitis. Some babies with myelomeningocele may develop an infection in the tissues surrounding the brain. This potentially dangerous infection may cause brain injury.
- Tethered spinal cord. A tethered spinal cord is when the spinal nerves attach to tissue and stretch. This can happen with scar tissue that resulted from surgery. When a spinal cord is tethered, it's less able to grow as the child grows. It can lead to loss of muscle function in the legs, bowel or bladder. Surgery can limit the degree of disability.
- Sleep-disordered breathing. Sleep apnea or other sleep conditions can affect both children and adults with spina bifida, particularly those with myelomeningocele. They may need to be tested to see if they briefly stop breathing several times during sleep, known as sleep apnea. Getting treatment can improve health and quality of life.
- Skin problems. Children with spina bifida have less feeling in some parts of their bodies and may get wounds on their feet, legs, buttocks or backs. Blisters or sores can turn into deep wounds or foot infections that are hard to treat. Children with myelomeningocele have a higher risk of developing wounds in casts.
- Latex allergy. Children with spina bifida have a higher risk of an allergic reaction to natural rubber or latex products. A latex allergy may cause rash, sneezing, itching, watery eyes and a runny nose. It also can cause a dangerous condition in which the face and airways swell and make it hard to breathe, known as anaphylaxis. It's best to use latex-free gloves and equipment during childbirth and when caring for a child with spina bifida.
- Other complications. Other medical issues may arise as children with spina bifida get older. These complications may include urinary tract infections, gastrointestinal (GI) conditions and depression. Children with myelomeningocele may have learning disabilities. They may have trouble paying attention and learning reading and math.
Prevention
You can greatly reduce your risk of having a baby with spina bifida or other neural tube defects by taking folic acid supplements. Begin taking the supplements at least one month before becoming pregnant and continue taking them through the first trimester of pregnancy.
Get folic acid first
Having enough folic acid in your body by the early weeks of pregnancy is critical to prevent spina bifida. But many people don't discover that they're pregnant until this time. For this reason, experts recommend that all people of childbearing age take a supplement of 400 micrograms (mcg) of folic acid a day.
It's also helpful to eat foods that contain folate or have had folic acid added to them, known as fortification. Foods that are fortified with folic acid include:
- Enriched bread.
- Pasta.
- Rice.
- Some breakfast cereals.
Folic acid may be listed on food packages as folate, which is the natural form of folic acid found in foods.
Planning pregnancy
Adults who are planning pregnancy or who could become pregnant need to get 400 to 800 mcg of folic acid a day.
The body doesn't absorb folate as easily as it absorbs folic acid, and most people don't get the recommended amount of folate through diet alone. Vitamin supplements that include folic acid are necessary to prevent spina bifida. It's also possible that folic acid may help lower the risk of other conditions that may be present at birth. These conditions include a cleft lip, a cleft palate and some heart conditions.
It's also a good idea to eat a healthy diet that includes foods rich in folate or fortified with folic acid. This vitamin is present naturally in many foods, including:
- Beans and peas.
- Citrus fruits and juices.
- Egg yolks.
- Cow's milk.
- Avocados.
- Dark green vegetables, such as broccoli and spinach.
When higher doses are needed
If you have spina bifida or if you've previously given birth to a child with spina bifida, you need extra folic acid before you become pregnant. If you're taking anti-seizure medicines or you have diabetes, you also may benefit from a higher dose of this B vitamin. Check with your healthcare professional before taking additional folic acid supplements.
Diagnosis
Tests before the birth of a baby, known as prenatal screening, can check for spina bifida and other conditions. The tests aren't perfect. Some people who have positive blood tests have babies without spina bifida. Even if the results are negative, there's still a small chance that spina bifida is present. Talk with your healthcare professional about prenatal testing, its risks and what the results mean.
Blood tests
Spina bifida can be screened with blood tests during pregnancy, but typically the diagnosis is made with an ultrasound exam.
- Maternal serum alpha-fetoprotein (MSAFP) test. For the MSAFP test, a sample of blood is drawn and tested for alpha-fetoprotein (AFP). This is a protein produced by the baby. It's typical for a small amount of AFP to cross the placenta and enter the pregnant parent's bloodstream. But high levels of AFP suggest that the baby may have a neural tube defect such as spina bifida. However, high levels of AFP don't always occur in spina bifida.
- Test to confirm high AFP levels. Varying levels of AFP can be caused by other factors such as a wrong estimate of the unborn baby's age or the presence of multiple babies. You may need a follow-up blood test to confirm the results. If levels of AFP are still high, you need further evaluation, including an ultrasound exam.
- Other blood tests. Your healthcare professional may perform the MSAFP test with two or three other blood tests. These tests screen for other conditions, such as trisomy 21 syndrome, also known as Down syndrome. They are commonly done with the MSAFP test.
Ultrasound
An ultrasound is the most accurate way to diagnose spina bifida in your baby before delivery. During pregnancy, an ultrasound may be done in the first 11 to 14 weeks of pregnancy, known as the first trimester. Or it may be done at 18 to 22 weeks, known as the second trimester. Spina bifida can be more accurately diagnosed during the second trimester ultrasound exam. This exam is crucial to identify and rule out conditions that may be present at birth.
An advanced ultrasound can detect symptoms of spina bifida, such as an open spine or features in the baby's brain. Sometimes ultrasound also can help your healthcare professional see how serious spina bifida is.
Amniocentesis
If the prenatal ultrasound confirms the diagnosis of spina bifida, your healthcare professional may request a test called amniocentesis. During this test, a needle is used to remove a sample of fluid from the amniotic sac that surrounds the baby. This exam may be important to rule out genetic diseases.
Talk to your healthcare professional about the potential risks of amniocentesis. There's a slight risk of loss of the pregnancy.
Treatment
Spina bifida treatment depends on how serious the condition is in your baby. Spina bifida occulta often doesn't need any treatment at all, but other types of spina bifida do.
Surgery before birth
Nerve function in babies with spina bifida can get worse if it's not treated. Prenatal surgery for spina bifida, also known as fetal surgery, takes place before the 26th week of pregnancy. Surgeons open the pregnant person's stomach and then the womb, also known as the uterus. The unborn baby's spinal cord is repaired. Then the surgeon closes the uterus and stomach. Sometimes this procedure can be done less invasively with a special surgical tool called a fetoscope. Instruments are inserted into the uterus through tiny ports to perform surgery on the unborn baby.
Research suggests that children with spina bifida who have fetal surgery may have less disability and be less likely to need crutches or other walking devices. Fetal surgery also may lower the risk of hydrocephalus. Ask your healthcare professional whether this procedure may be right for you. Ask about the potential benefits. Also ask about the risks to you and your baby, such as premature delivery and other complications.
It's important to have a comprehensive evaluation to determine whether fetal surgery can be done. This specialized surgery should only be done at a healthcare facility with experienced fetal surgery experts, a multispecialty team and neonatal intensive care. Typically, the team includes a fetal surgeon, a pediatric neurosurgeon, a maternal-fetal medicine specialist, a fetal cardiologist and a neonatologist.
Cesarean birth
Many babies with myelomeningocele tend to be in a feet-first position, known as breech. Cesarean birth may be a safer way to deliver if your baby is breech or has a large cyst or sac.
Surgery after birth
Myelomeningocele requires surgery to close the opening in the baby's back within 72 hours of birth. Early surgery can help lower the risk of infection associated with the exposed nerves. It also may help protect the spinal cord from more trauma.
During the procedure, a neurosurgeon places the spinal cord and exposed tissue inside the baby's body and covers them with muscle and skin. At the same time, the neurosurgeon may place a shunt in the baby's brain to control hydrocephalus.
Treatment for complications
In babies with myelomeningocele, nerve damage that can't be repaired has likely already occurred in the uterus. Ongoing care from a multispecialty team of surgeons, physicians and therapists usually is needed. Babies with myelomeningocele may need more surgery for complications. Complications can include weak legs, bladder and bowel issues, or hydrocephalus. Treatment typically begins soon after birth.
Treatment options may include:
- Walking and mobility aids. Some babies may start exercises to prepare their legs for walking with braces or crutches when the babies are older. Some children may need walkers or a wheelchair. Mobility aids, along with regular physical therapy, can help a child become independent. Even children who need a wheelchair can learn to function well and become self-sufficient.
-
Bowel and bladder management. Routine bowel and bladder evaluations and management help reduce the risk of organ damage and illness. Evaluations include X-rays, kidney scans, ultrasounds, blood tests and bladder function studies. These evaluations are more frequent in the first few years of life and are done less often as children grow. A specialist in pediatric urology with experience in performing surgery on children with spina bifida may offer the most effective management options.
Bowel management may include oral medicines, suppositories, enemas, surgery or a combination of these approaches. Bladder management may include medicines, catheters to empty the bladder, surgery or a combination of treatments.
-
Surgery for hydrocephalus. Most babies with myelomeningocele need surgery to place a tube that allows fluid in the brain to drain into another part of the body. The tube is called a ventricular shunt. It may be placed just after birth, during the surgery to close the sac on the back. Or it may be placed later as fluid builds up.
A less invasive procedure called endoscopic third ventriculostomy is an option for some babies. But certain criteria must be met before this procedure is done. The surgeon uses a small video camera to see inside the brain. The surgeon then makes a hole in the bottom of or between brain cavities. This allows cerebrospinal fluid to flow out of the brain.
- Treatment and management of other complications. Special equipment such as bath chairs, commode chairs and standing frames may help with daily functioning. Most spina bifida complications can be treated or managed to improve quality of life. These include orthopedic complications, a tethered spinal cord, GI issues, skin conditions and other complications.
Ongoing care
Children with spina bifida need close follow-up care and observation. Their healthcare professionals evaluate their growth, the need for vaccinations and general medical issues. Medical care is coordinated among specialists.
Children with spina bifida often need treatment and ongoing care from healthcare professionals with expertise in:
- Physical medicine and rehabilitation.
- Neurology.
- Neurosurgery.
- Urology.
- Orthopedics.
- Physical therapy.
- Occupational therapy.
- Special education.
- Social work.
- Nutrition.
Parents and other caregivers are a key part of the team. They can learn how to help manage a child's condition and how to encourage and support the child emotionally and socially.
Coping and support
News that your newborn child has a condition such as spina bifida can naturally cause you to feel many emotions. It's important to know that people with spina bifida live active, productive and full lives — especially with encouragement and support from loved ones. Children with spina bifida can go to college, hold jobs and have families.
Special accommodations may be necessary along the way. But encourage your child to be as independent as possible.
Independent mobility is an important and appropriate goal for all children with spina bifida. This may mean walking with or without braces, using walking aids such as canes or crutches, or using a wheelchair. Encourage your child to engage in activities with peers. Caregivers can help adjust activities to accommodate physical disabilities.
Many children with spina bifida have typical intelligence, but some may need educational help for learning disabilities. They may have trouble with attention, concentration or language that requires treatment from professionals outside of school.
As for any child with a chronic medical condition, children with spina bifida may benefit from meeting with mental health professionals. A child psychologist and other mental health professionals can help with adjustment and coping. Most children with spina bifida are resilient and adapt to their challenges with support from their parents, teachers and other caregivers.
If your child has spina bifida, you may benefit from finding a support group of other parents who are dealing with the condition. Talking with others who understand the challenges of living with spina bifida can be helpful.
Preparing for an appointment
Your healthcare professional may suspect or diagnose your baby's condition during your pregnancy. You'll likely consult with a multispecialty team of physicians, surgeons and physical therapists at a center that specializes in spina bifida treatment.
Here's some information to help you get ready for your appointment and know what to expect.
What you can do
To prepare for the appointment:
- Be aware of any pre-appointment instructions. At the time you make the appointment, be sure to ask if there's anything you need to do in advance. For example, you might need to drink extra water before an ultrasound.
- Make a list of all medicines, vitamins, herbs and supplements that you took before and during your pregnancy, and how much.
- Ask a family member or friend to come with you, if possible. Sometimes it can be hard to remember all the information provided to you during an appointment. Someone who comes with you may remember something that you missed or forgot.
- Create a list of questions to ask, starting with the most important.
For spina bifida, some basic questions to ask include:
- Is spina bifida present and how serious is it?
- Is there evidence of a buildup of fluid in my baby's brain?
- Can my baby be treated during pregnancy?
- What will be done for my baby immediately after birth?
- Will the treatment cure my child?
- Will there be any lasting effects?
- Who can I contact to find out about community resources that may be able to help my child?
- What is the likelihood of this happening again in future pregnancies?
- How can I keep this from happening again in the future?
- Are there any brochures or other printed material that I can have? What websites do you recommend?
In addition to the questions that you've prepared, don't hesitate to ask other questions during your appointment.
What to expect from your doctor
Being ready to answer questions from your healthcare professional may give you time to go over any points you want to focus on. You may be asked:
- Have you ever had a child with spina bifida or other conditions at birth?
- Is there a family history of spina bifida?
- Did you take folic acid, also known as vitamin B-9, before and during your pregnancy?
- Are you taking any anti-seizure medicines, or were you taking them at the beginning of your pregnancy?
- If necessary, are you able to travel to a facility that offers specialized care?
Last Updated Dec 19, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use




