Coronary angiogram
Overview
A coronary angiogram is a test that uses X-rays to look at the heart's blood vessels, called the coronary arteries. It's usually done to see if a blood vessel is narrowed or blocked. A coronary angiogram is most often used to diagnose coronary artery disease.
A coronary angiogram is part of a general group of heart tests and treatments called cardiac catheterization. Cardiac catheterization uses one or more thin, flexible tubes, called catheters. The tubes are placed within the major blood vessels of the body and the heart. The test requires a small cut in the skin. During a coronary angiogram, a treatment called angioplasty and stenting can be done to open any blocked arteries.
Sometimes, a computerized tomography (CT) machine is used to look at the heart's blood vessels. This type of angiogram doesn't need tubes placed inside the body. It's called a coronary CT angiogram (CCTA). It may be done to determine whether someone needs cardiac catheterization. A narrowing or blockage in the vessels cannot be treated during a CT angiogram. If the test shows a blocked or narrowed artery, the catheter type of coronary angiogram must be done.
This article focuses on coronary angiogram with cardiac catheterization.
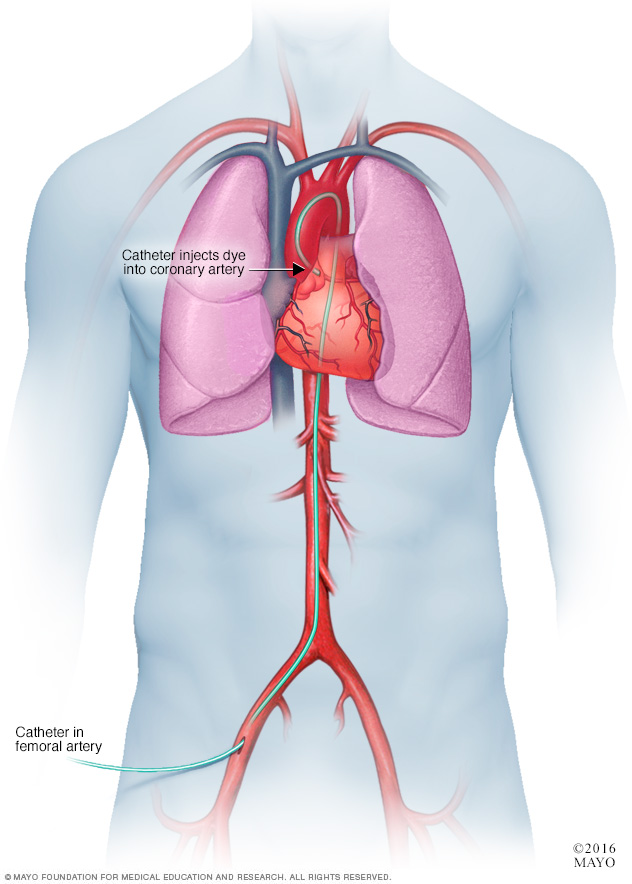
In a coronary angiogram, a flexible tube called a catheter is inserted into an artery, usually in the groin, arm or neck. It's guided to the heart. A coronary angiogram can show blocked or narrowed blood vessels in the heart.
Why it's done
A coronary angiogram is done to look for narrowed or blocked blood vessels in the heart.
Your healthcare team may suggest a coronary angiogram if you have:
- Chest pain, called angina.
- Pain in the chest, jaw, neck or arm that can't be explained by other tests.
- Blood vessel problems.
- A heart problem you were born with, called a congenital heart defect.
- Irregular results on an exercise stress test.
- Chest injury.
- Heart valve disease that needs surgery.
An angiogram typically is not done until other noninvasive tests are used to check the heart. Such tests might include an electrocardiogram, an echocardiogram or a stress test.
Risks
A coronary angiogram involves the blood vessels and heart, so there are some risks. But major complications are rare. Possible risks and complications may include:
- Blood vessel injury.
- Excessive bleeding.
- Heart attack.
- Infection.
- Irregular heart rhythms, called arrhythmias.
- Kidney damage due to the dye used during the test.
- Reactions to the dye or medicines used during the test.
- Stroke.
How you prepare
Sometimes, a coronary angiogram is done in an emergency. There may not be time to prepare. When the test is scheduled in advance, your healthcare team gives you instructions on how to prepare.
General guidelines typically include these instructions:
- Do not eat or drink anything for several hours before the test. Your care team tells you what time you need to stop eating and drinking.
- Ask if you can take your regular medicines. Take a list of your medicines with you to the hospital. Include their dosages.
- Tell your care team if you have diabetes. You may need insulin or another medicine before a coronary angiogram.
What you can expect
Before the procedure
A coronary angiogram is done in a hospital or medical center in a room called a catheterization laboratory. It's often called a cath lab. Before the test, your healthcare team talks to you about the medicines you take and your allergies.
You change into a hospital gown and empty your bladder, if needed. Do not wear contact lenses, eyeglasses, jewelry or hairpins.
The care team checks your blood pressure and pulse. Sticky patches, called electrodes, are placed on your chest and sometimes the arms or legs. The patches record your heartbeat. They stay on for the entire test and for a while after.
A healthcare professional may shave a small amount of hair from the area where a flexible tube, called a catheter, will be inserted. The area is cleaned and then numbed.
During the procedure
During a coronary angiogram, you lie on your back on a table. Straps go across your chest and legs to keep you safely on the table.
A healthcare professional places an IV into a vein in your forearm or hand. Medicine called a sedative goes through the IV. The medicine helps you feel relaxed and calm during the test or treatment. It may make you feel sleepy.
The amount of sedation you need depends on the reason for the coronary angiogram and your overall health. You may be fully awake or lightly sedated. Or you may be given a combination of medicines to put you in a sleep-like state. This is called general anesthesia.
The doctor makes a small cut, called an incision, to reach an artery. This cut may be made in the leg or wrist. A thin, flexible tube called a catheter is placed in the artery and guided to the heart. You shouldn't feel it moving through your body.
Once the catheter is in the correct position, dye flows through the tube into the heart's blood vessels. X-ray images are taken to see how the dye moves. These images are called angiograms. If the dye doesn't move through a blood vessel, it could mean the area is blocked or narrowed.
An uncomplicated coronary angiogram may take an hour or longer to complete. It depends on whether other heart tests or treatments are done at the same time. If a blockage is found, a balloon may be passed through the catheter and expanded to widen the artery. A mesh tube called a stent may be placed to keep the artery open.
When the test or treatment is done, the catheter is removed from the body. A clamp or small plug may be used to close the small incision.
After the procedure
After a coronary angiogram, you are taken to a recovery area. A healthcare team watches you and checks your heartbeat, blood pressure and oxygen levels.
If the catheter was placed in the leg area, you must lie flat for several hours. This helps prevent bleeding. The area where the catheter was placed may feel sore for a while. You may have a bruise and a small bump.
Some people go home the same day after having a coronary angiogram. Others stay in the hospital for a day or more, depending on the results of the test.
As you recover, follow these general tips:
- Drink plenty of fluids to help flush the dye from your body.
- Avoid strenuous exercise and heavy lifting for several days.
- Ask your healthcare team when you can bathe and shower.
- Take your medicines as directed by your care team.
Your care team tells you when you can return to work and daily activities.
Call your healthcare professional's office if you have:
- Chest pain or shortness of breath.
- Bleeding, new bruising, swelling or increasing pain at the catheter site.
- Symptoms of infection, such as a fever.
- Drainage or a change in color around the incision. This may be a shade of red, purple or brown depending on your skin color.
- A change in temperature or color of the leg or arm that was used for the test.
- Weakness or numbness in a leg or arm.
Call 911 or your local emergency number if the area where the catheter was placed keeps bleeding and doesn't stop with pressure.
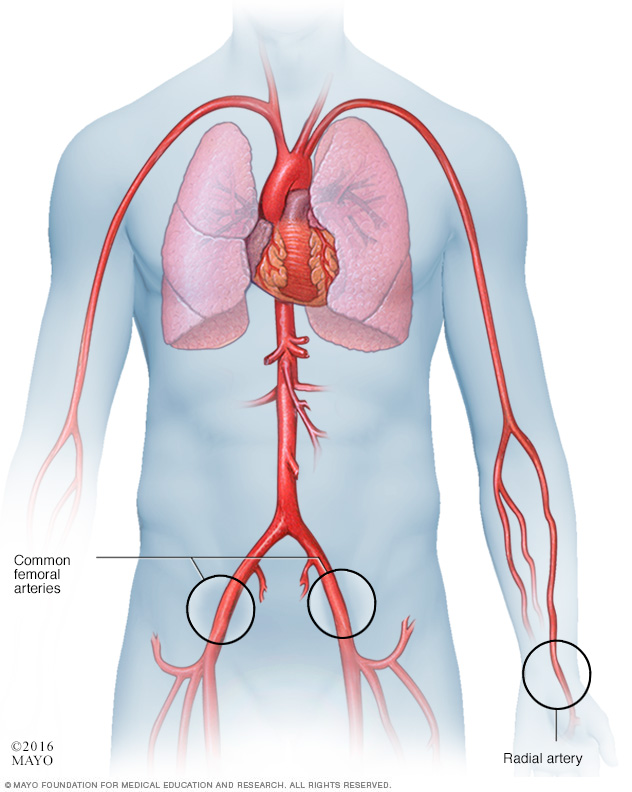
In a cardiac catheter procedure, a doctor inserts a flexible tube called a catheter into a blood vessel. Sometimes it's placed in the wrist artery, called the radial artery. Or it may be placed in an artery in the groin, called the femoral artery. The catheter is then guided to the heart.
Results
A coronary angiogram shows how blood flows through the heart arteries. A healthcare professional can use the test results to do the following:
- Identify a blocked or narrowed artery.
- Learn how much blood flow to or from the heart is reduced.
- Determine if there's a buildup of fats, cholesterol and other substances in and on the artery walls, a condition called atherosclerosis.
- Check the results of previous heart surgery.
Knowing this information helps your care team plan the best treatment for your condition.
Last Updated Dec 6, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use





