Graves' disease
Overview
Graves' disease is an immune system condition that affects the thyroid gland. It causes the body to make too much thyroid hormone. That condition is called hyperthyroidism.
Thyroid hormones affect many organs in the body. So Graves' disease symptoms also can affect those organs. Anyone can get Graves' disease. But it's more common in women and in people older than 30.
Treatment for Graves' disease helps lower the amount of thyroid hormone that the body makes and eases symptoms.
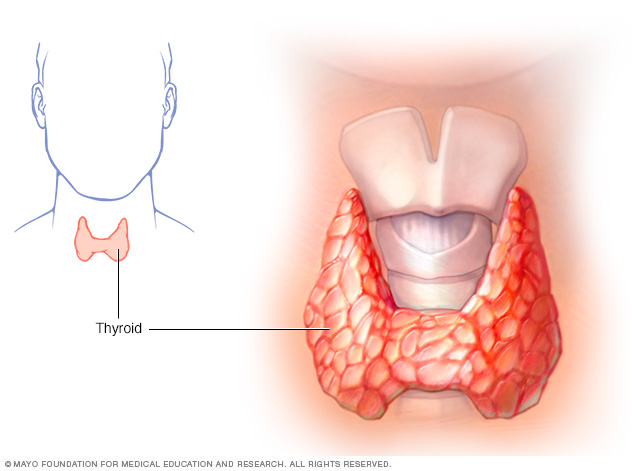
The thyroid gland sits at the base of the neck.
Symptoms
Common symptoms of Graves' disease include:
- Feeling nervous and irritable.
- Having a slight tremor of the hands or fingers.
- Being sensitive to heat with an increase in sweating or warm, moist skin.
- Losing weight, despite wanting to eat more.
- Having an enlarged thyroid gland, also called goiter.
- Having changes in menstrual cycles.
- Not being able to get or keep an erection, called erectile dysfunction, or having less desire for sex.
- Having bowel movements often.
- Having bulging eyes — a condition called thyroid eye disease or Graves' ophthalmopathy.
- Being tired.
- Having thick, discolored skin mostly on the shins or tops of the feet, called Graves' dermopathy.
- Having fast or irregular heartbeat, called palpitations.
- Not sleeping well.
Thyroid eye disease
Thyroid eye disease also is called Graves' ophthalmopathy. About 25% of people with Graves' disease have eye symptoms. Thyroid eye disease affects muscles and other tissues around the eyes. Symptoms may include:
- Bulging eyes.
- A gritty feeling in the eyes.
- Pressure or pain in the eyes.
- Puffy eyelids or eyelids that don't cover the eyeball all the way. This is called retracted eyelids.
- Red or inflamed eyes.
- Light sensitivity.
- Blurred or double vision.
- Vision loss.
Graves' dermopathy
Rarely, people with Graves' disease have darkening and thickening of the skin. It most often appears on the shins or the tops of the feet. The skin has a texture like an orange peel.
This is called Graves' dermopathy. It comes from a buildup of protein in the skin. It's most often mild and painless.
When to see a doctor
Other medical conditions can cause symptoms like those of Graves' disease. See your healthcare professional if you have any symptoms of Graves' disease to get a prompt diagnosis.
Seek medical care right away if you have heart-related symptoms, such as a fast or irregular heartbeat, or if you have vision loss.
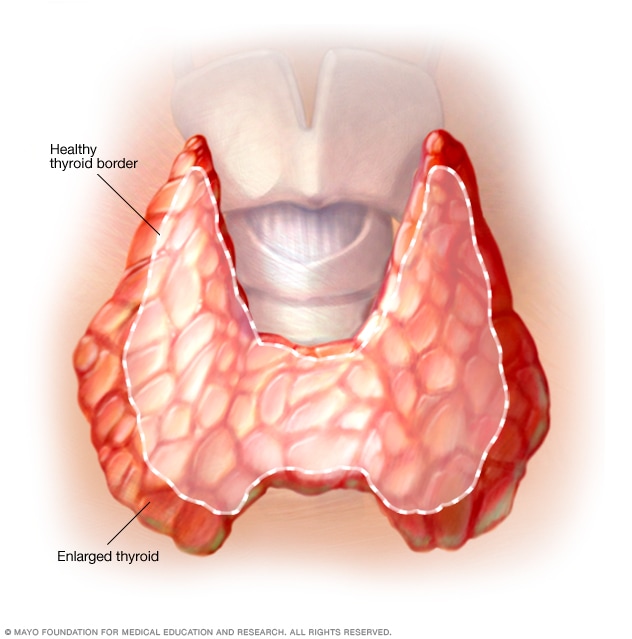
An enlarged thyroid can cause a bulge in the neck.
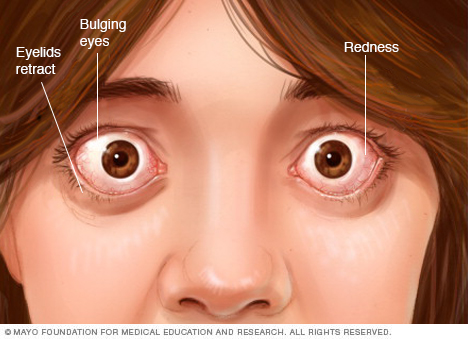
Thyroid eye disease symptoms include bulging eyes and redness. The eyelids may not cover the eyeball all the way. This eye condition also is called Graves' ophthalmopathy.
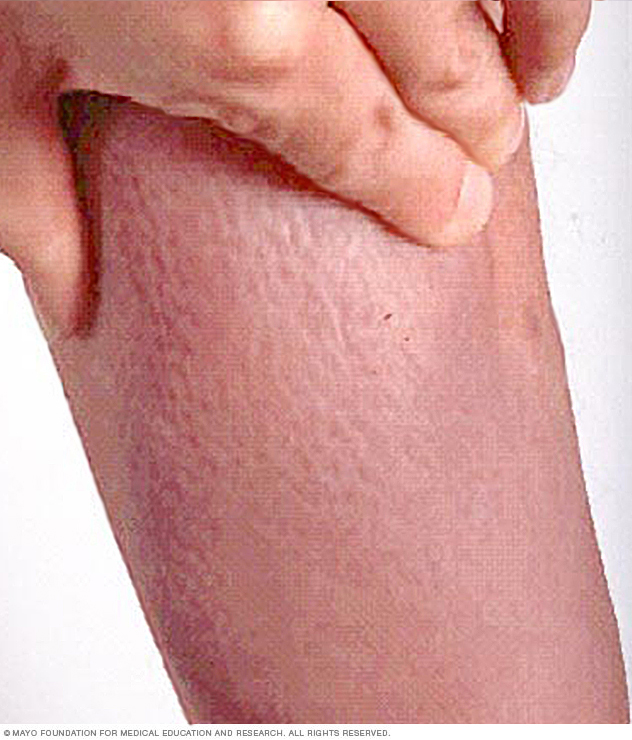
Rarely, people who have Graves' disease have skin that darkens and thickens. The skin has a texture like an orange peel. This is called Graves' dermopathy. It comes from a buildup of protein in the skin. It often appears on the shins and on the tops of the feet.
Causes
Graves' disease is caused by the body's disease-fighting immune system not working correctly. Experts don't know why this happens.
The immune system makes antibodies that target viruses, bacteria or other foreign substances. In Graves' disease, the immune system makes an antibody to one part of the cells in the hormone-making gland in the neck, called the thyroid gland.
A tiny gland at the base of the brain, called the pituitary gland, makes a hormone that controls the thyroid gland. The antibody linked with Graves' disease is called thyrotropin receptor antibody (TRAb). TRAb takes over the work of the pituitary hormone. That leads to more thyroid hormone in the body than the body needs. That condition is called hyperthyroidism.
Cause of thyroid eye disease
Thyroid eye disease, also called Graves' ophthalmopathy, comes from a buildup of certain carbohydrates in the muscles and tissues behind the eyes. The cause isn't known. It may involve the same antibody that can cause the thyroid gland to not work correctly.
Thyroid eye disease often appears at the same time as hyperthyroidism or several months later. But symptoms of thyroid eye disease can appear years before or after hyperthyroidism starts. It's also possible to have thyroid eye disease without hyperthyroidism.
Risk factors
Factors that can increase the risk of Graves' disease include:
- Family history. People who get Graves' disease often have a family history of thyroid conditions or an autoimmune condition.
- Sex. Women are much more likely to get Graves' disease than are men.
- Age. Graves' disease mostly happens between the ages of 30 and 60.
- Another autoimmune condition. People with other conditions of the immune system, such as type 1 diabetes or rheumatoid arthritis, have a higher risk.
- Smoking. Cigarette smoking, which can affect the immune system, raises the risk of Graves' disease. People who smoke and have Graves' disease are at higher risk of getting thyroid eye disease.
Complications
Complications of Graves' disease can include:
- Pregnancy health concerns. Graves' disease during pregnancy can cause miscarriage, early birth, fetal thyroid issues and poor fetal growth. It also can cause heart failure and preeclampsia in the pregnant person. Preeclampsia leads to high blood pressure and other serious symptoms.
- Heart conditions. Graves' disease that isn't treated can lead to irregular heart rhythms and changes in the heart and how it works. The heart might not be able to pump enough blood to the body. That condition is called heart failure.
-
Thyroid storm. This rare but deadly complication of Graves' disease also is called accelerated hyperthyroidism or thyrotoxic crisis. It's more likely to happen when severe hyperthyroidism is not treated or not treated well enough.
Thyroid storm happens when a sudden and drastic rise in thyroid hormones causes a number of effects in the body. They include fever, sweating, confusion, delirium, severe weakness, tremors, irregular heartbeat, severe low blood pressure and coma. Thyroid storm needs medical attention right away.
- Brittle bones. Hyperthyroidism that isn't treated can lead to weak, brittle bones — a condition called osteoporosis. The strength of the bones depends, in part, on the amount of calcium and other minerals they hold. Too much thyroid hormone makes it hard for the body to get calcium into the bones.
Diagnosis
To diagnose Graves' disease, your healthcare professional may do a physical exam and ask about your medical and family history. Tests might include:
-
Blood tests. Blood tests show the levels of thyroid-stimulating hormone (TSH) and thyroid hormones in the body. TSH is the pituitary hormone that spurs the thyroid gland. People with Graves' disease most often have lower than usual levels of TSH and higher levels of thyroid hormones.
Another lab test measures the levels of the antibody known to cause Graves' disease. If the results don't show antibodies, there might be another cause of hyperthyroidism.
-
Radioactive iodine uptake. The body needs iodine to make thyroid hormones. This test involves taking a small amount of radioactive iodine. Later, a special scanning camera shows how much of the iodine gets into the thyroid gland. This test can show how fast the thyroid gland takes up iodine.
The amount of radioactive iodine the thyroid gland takes up helps show whether Graves' disease or another condition is the cause of the hyperthyroidism. This test may be used with a radioactive iodine scan to show a picture of the uptake pattern.
Treatment
Treatment for Graves' disease aims to stop the thyroid from making hormones. Treatment also blocks the effect of the hormones on the body.
Radioactive iodine therapy
With this therapy, you take radioactive iodine, called radioiodine, by mouth. The radioiodine goes into the thyroid cells. Over time, it destroys the cells that make thyroid hormone. This causes your thyroid gland to shrink. Symptoms ease little by little, most often over several weeks to several months.
Radioiodine therapy may raise the risk of thyroid eye disease or make its symptoms worse. This side effect most often is mild and doesn't last. But the therapy might not be for you if you have moderate to severe eye symptoms.
Other side effects may include a tender neck and a brief rise in thyroid hormones. Radioiodine therapy isn't used for treating pregnant people or those who are breastfeeding.
This treatment destroys cells that make thyroid hormone. After the treatment, you'll likely need to take daily hormone medicine to get the thyroid hormones your body needs.
Anti-thyroid medicines
Anti-thyroid medicines block the thyroid from using iodine to make hormones. These prescription medicines include propylthiouracil and methimazole.
Because the risk of liver failure is more common with propylthiouracil, methimazole is most often the first choice. But methimazole has a slight risk of birth defects. So propylthiouracil might be prescribed during the first trimester of pregnancy. Pregnant people typically take methimazole after the first trimester.
When either of these medicines are used without other treatments, hyperthyroidism may come back. These medicines may work better when they are taken for longer than a year. Anti-thyroid medicines may be used before or after radioiodine therapy as an added treatment.
Side effects of both medicines include rash, joint pain, liver failure or a decrease in disease-fighting white blood cells.
Beta blockers
These medicines don't stop the body from making thyroid hormones. But they block the effect of hormones on the body. They may work quickly to ease irregular heartbeats, tremors, anxiety, irritability, heat intolerance, sweating, diarrhea and muscle weakness.
Beta blockers include:
- Propranolol (Inderal LA, InnoPran XL, Hemangeol).
- Atenolol (Tenormin).
- Metoprolol (Lopressor, Toprol-XL).
- Nadolol (Corgard).
Beta blockers aren't often given to people with asthma because they can cause an asthma attack. These medicines also might make it harder to manage diabetes.
Surgery
Surgery to remove the thyroid, called thyroidectomy, can treat Graves' disease. You need to take thyroid medicine for the rest of your life after this surgery.
Risks of this surgery include damage to the nerve that controls the vocal cords and damage to the tiny glands that sit next to the thyroid gland, called the parathyroid glands. The parathyroid glands make a hormone that controls the level of calcium in the blood. Complications are rare with surgeons who have done a lot of thyroid surgeries.
Treating thyroid eye disease
For mild symptoms of thyroid eye disease, using artificial tears during the day may be helpful. You can buy artificial tears without a prescription. Use lubricating gels at night.
For symptoms of thyroid eye disease that are worse, treatment might include:
- Corticosteroids. Treatment with corticosteroids given through a vein may ease swelling behind the eyeballs. Side effects might include fluid buildup, weight gain, high blood sugar, high blood pressure and mood swings.
- Teprotumumab (Tepezza). This medicine is given eight times. It's given through an IV in the arm every three weeks. It can cause side effects such as hearing loss, nausea, diarrhea, muscle spasms and high blood sugar.
- Prisms. You may have double vision either because of Graves' disease or as a side effect of surgery for Graves' disease. Though they don't work for everyone, prisms in your glasses may correct double vision.
-
Orbital decompression surgery. In this surgery, a surgeon removes the bone between the eye socket, called the orbit, and the air spaces next to the orbit, called the sinuses. This gives the eyes room to move back to their usual place.
This treatment is mainly used if pressure on the optic nerve might cause loss of vision. Possible complications include double vision.
- Orbital radiotherapy. This was once a common treatment for thyroid eye disease, but how it helps isn't clear. It uses X-rays over several days to destroy some of the tissue behind the eyes. Your healthcare professional might suggest this treatment if your eye problems are getting worse and corticosteroids aren't working, or they cause too many side effects.
Thyroid eye disease doesn't always get better with treatment of Graves' disease. Symptoms of thyroid eye disease may even get worse for 3 to 6 months. After that, the symptoms of thyroid eye disease most often stay the same for a year or so. Then the symptoms begin to get better, often on their own.
Lifestyle and home remedies
If you have Graves' disease, it's important to take care of your mental and physical health. This includes:
-
Eating well and exercising. These can help ease some symptoms during treatment and help you feel better overall. Your thyroid controls how you burn calories. So you may gain weight when the hyperthyroidism is corrected.
Brittle bones also can happen with Graves' disease. Weight-bearing exercises can help keep bones strong.
- Easing stress. Stress can trigger Graves' disease or make it worse. Listening to music, taking a warm bath or walking can help you relax and put you in a better mood.
Work with your healthcare team to design a plan that makes eating well, exercising and relaxing part of each day.
Thyroid eye disease
For thyroid eye disease, also called Graves' ophthalmopathy, these steps may help:
- Put cool, damp cloths on your eyes. This can soothe your eyes.
- Wear sunglasses. Ultraviolet rays and bright lights can affect your eyes more if they bulge. Wearing sunglasses that wrap around the sides of your head can help. And they also can keep wind from bothering your eyes.
- Use lubricating eye drops. Eye drops may relieve the dry, scratchy feeling of your eyes. Try a lubricating gel at night.
- Raise the head of your bed. Keeping your head higher than the rest of your body lessens fluid buildup in the head and may ease the pressure on your eyes.
- Tape shut the eyelids. If your eyelids don't close all the way, taping them shut during sleep or wearing a sleep mask might help.
- Don't smoke. Smoking worsens thyroid eye disease.
Graves' dermopathy
If Graves' disease affects your skin, use creams or ointments that have hydrocortisone. You can buy these without a prescription. The hydrocortisone can ease swelling. Using compression wraps on your legs also may help.
Preparing for an appointment
You likely will start by seeing your primary healthcare professional. You may then be sent to a specialist in hormones and the endocrine system, called an endocrinologist. If you have thyroid eye disease, you also might be sent to an eye specialist, called an ophthalmologist.
Here's some information to help you get ready for your appointment.
What you can do
Make a list of:
- Your symptoms, even ones that don't seem related, and when they began.
- Key personal information, including your family medical history and recent stresses or life changes.
- All medicines, vitamins or supplements that you take, including doses.
- Questions to ask your healthcare team.
For Graves' disease, questions might include:
- What's the most likely cause of my symptoms?
- What tests do I need? Do I need to prepare for any of these tests?
- Is this condition likely to be brief or long lasting?
- What treatments are there. Which do you suggest?
- What side effects can I expect from treatment?
- I have other health conditions. How can I best manage these conditions together?
- Where can I find more information on Graves' disease?
What to expect from your doctor
Your healthcare team is likely to ask you questions, such as:
- Do you have symptoms all the time or do they come and go?
- Have you recently started a new medicine?
- Have you lost weight quickly or without trying? How much have you lost?
- Have you had any change in your menstrual cycle?
- Have you had sexual problems?
- Do you have trouble sleeping?
Last Updated Jun 14, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



