Heart disease
Overview
Heart disease describes a range of conditions that affect the heart. Heart diseases include:
- Blood vessel disease, such as coronary artery disease
- Irregular heartbeats (arrhythmias)
- Heart problems you're born with (congenital heart defects)
- Disease of the heart muscle
- Heart valve disease
Many forms of heart disease can be prevented or treated with healthy lifestyle choices.
Symptoms
Heart disease symptoms depend on the type of heart disease.
Symptoms of heart disease in the blood vessels
Coronary artery disease is a common heart condition that affects the major blood vessels that supply the heart muscle. Cholesterol deposits (plaques) in the heart arteries are usually the cause of coronary artery disease. The buildup of these plaques is called atherosclerosis (ath-ur-o-skluh-ROE-sis). Atherosclerosis reduces blood flow to the heart and other parts of the body. It can lead to a heart attack, chest pain (angina) or stroke.
Coronary artery disease symptoms may be different for men and women. For instance, men are more likely to have chest pain. Women are more likely to have other symptoms along with chest discomfort, such as shortness of breath, nausea and extreme fatigue.
Symptoms of coronary artery disease can include:
- Chest pain, chest tightness, chest pressure and chest discomfort (angina)
- Shortness of breath
- Pain in the neck, jaw, throat, upper belly area or back
- Pain, numbness, weakness or coldness in the legs or arms if the blood vessels in those body areas are narrowed
You might not be diagnosed with coronary artery disease until you have a heart attack, angina, stroke or heart failure. It's important to watch for heart symptoms and discuss concerns with your health care provider. Heart (cardiovascular) disease can sometimes be found early with regular health checkups.
Heart disease symptoms caused by irregular heartbeats (heart arrhythmias)
The heart may beat too quickly, too slowly or irregularly. Heart arrhythmia symptoms can include:
- Chest pain or discomfort
- Dizziness
- Fainting (syncope) or near fainting
- Fluttering in the chest
- Lightheadedness
- Racing heartbeat (tachycardia)
- Shortness of breath
- Slow heartbeat (bradycardia)
Heart disease symptoms caused by congenital heart defects
Serious congenital heart defects usually are noticed soon after birth. Congenital heart defect symptoms in children could include:
- Pale gray or blue skin or lips (cyanosis)
- Swelling in the legs, belly area or areas around the eyes
- In an infant, shortness of breath during feedings, leading to poor weight gain
Less-serious congenital heart defects are often not diagnosed until later in childhood or during adulthood. Symptoms of congenital heart defects that usually aren't immediately life-threatening include:
- Easily getting short of breath during exercise or activity
- Easily tiring during exercise or activity
- Swelling of the hands, ankles or feet
Heart disease symptoms caused by diseased heart muscle (cardiomyopathy)
Early stages of cardiomyopathy may not cause noticeable symptoms. As the condition worsens, symptoms may include:
- Dizziness, lightheadedness and fainting
- Fatigue
- Feeling short of breath during activity or at rest
- Feeling short of breath at night when trying to sleep or waking up short of breath
- Irregular heartbeats that feel rapid, pounding or fluttering
- Swollen legs, ankles or feet
Heart disease symptoms caused by heart valve problems (valvular heart disease)
The heart has four valves — the aortic, mitral, pulmonary and tricuspid valves. They open and close to move blood through the heart. Many things can damage the heart valves. A heart valve may become narrowed (stenosis), leaky (regurgitation or insufficiency) or close improperly (prolapse).
Valvular heart disease is also called heart valve disease. Depending on which valve isn't working properly, heart valve disease symptoms generally include:
- Chest pain
- Fainting (syncope)
- Fatigue
- Irregular heartbeat
- Shortness of breath
- Swollen feet or ankles
Endocarditis is an infection that affects the heart valves and inner lining of the heart chambers and heart valves (endocardium). Endocarditis symptoms can include:
- Dry or persistent cough
- Fever
- Heartbeat changes
- Shortness of breath
- Skin rashes or unusual spots
- Swelling of the legs or belly area
- Weakness or fatigue
When to see a doctor
Seek emergency medical care if you have these heart disease symptoms:
- Chest pain
- Shortness of breath
- Fainting
Always call 911 or emergency medical help if you think you might be having a heart attack.
Heart disease is easier to treat when detected early. Talk to your health care provider if you have any concerns about your heart health. Together, you and your provider can discuss ways to reduce your heart disease risk. This is especially important if you have a family history of heart disease.
If you think you may symptoms of heart disease, make an appointment to see your provider.
Causes
Heart disease causes depend on the specific type of heart disease. There are many different types of heart disease.
How the heart works
To understand the causes of heart disease, it may help to understand how the heart works.
- The heart is divided into chambers — two upper chambers (atria) and two lower chambers (ventricles).
- The right side of the heart moves blood to the lungs through blood vessels (pulmonary arteries).
- In the lungs, blood picks up oxygen and then returns to the left side of the heart through the pulmonary veins.
- The left side of the heart then pumps the blood through the aorta and out to the rest of the body.
Heart valves
Four heart valves — the aortic, mitral, pulmonary and tricuspid — keep the blood moving the right way. The valves open only one way and only when they need to. Valves must open all the way and close tightly so there's no leakage.
Heartbeats
A beating heart squeezes (contracts) and relaxes in a continuous cycle.
- During contraction (systole), the lower heart chambers (ventricles) squeeze tight. This action forces blood to the lungs and the rest of the body.
- During relaxation (diastole), the ventricles fill with blood from the upper heart chambers (atria).
Electrical system
The heart's electrical system keeps it beating. The heartbeat controls the continuous exchange of oxygen-rich blood with oxygen-poor blood. This exchange keeps you alive.
- Electrical signals start in the upper right chamber (right atrium).
- The signals travel through specialized pathways to the lower heart chambers (ventricles). This tells the heart to pump.
Causes of coronary artery disease
A buildup of fatty plaques in the arteries (atherosclerosis) is the most common cause of coronary artery disease. Risk factors include a poor diet, lack of exercise, obesity and smoking. Healthy lifestyle choices can help lower the risk of atherosclerosis.
Causes of irregular heartbeats (arrhythmias)
Common causes of arrhythmias or conditions that can lead to them include:
- Cardiomyopathy
- Coronary artery disease
- Diabetes
- Drug misuse
- Emotional stress
- Excessive use of alcohol or caffeine
- Heart problem present at birth (congenital heart defects)
- High blood pressure
- Smoking
- Heart valve disease
- Use of certain medications, including those bought without a prescription, and herbs and supplements
Causes of congenital heart defects
A congenital heart defect develops while a baby is growing in the womb. A congenital heart defect forms as the baby's heart develops, about a month after conception. Congenital heart defects change the flow of blood in the heart. Some medical conditions, medications and genes increase the risk of congenital heart defects.
Causes of a thickened or enlarged heart muscle (cardiomyopathy)
The cause of cardiomyopathy depends on the type:
- Dilated cardiomyopathy. The cause of this most common type of cardiomyopathy often is unknown. It may be passed down through families (inherited). Dilated cardiomyopathy typically starts in the heart's main pumping chamber (left ventricle). Many things can cause damage to the left ventricle, including heart attacks, infections, toxins and some drugs, including cancer medicines.
- Hypertrophic cardiomyopathy. This type is usually passed down through families (inherited).
- Restrictive cardiomyopathy. This is the least common type of cardiomyopathy. It can occur for no known reason. Sometimes it's caused by a buildup of protein called amyloid in the heart (cardiac amyloidosis) or connective tissue disorders.
Causes of heart infection
A heart infection, such as endocarditis, occurs when germs reach the heart or heart valves. The most common causes of heart infections are:
- Bacteria
- Viruses
- Parasites
Causes of heart valve disease
Many things can cause diseases of the heart valves. Some people are born with heart valve disease (congenital heart valve disease). Heart valve disease may also be caused by conditions such as:
- Rheumatic fever
- Infections (infectious endocarditis)
- Connective tissue disorders
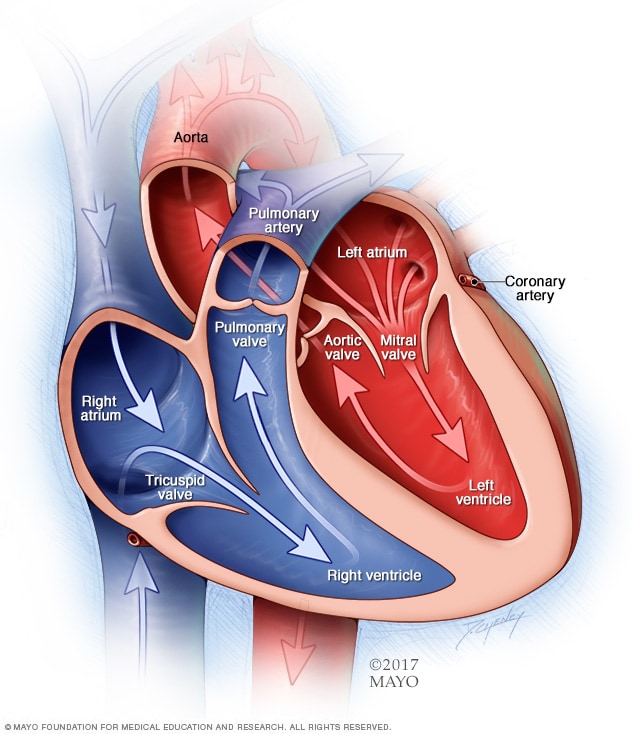
A typical heart has two upper and two lower chambers. The upper chambers, the right and left atria, receive incoming blood. The lower chambers, the more muscular right and left ventricles, pump blood out of the heart. The heart valves are gates at the chamber openings. They keep blood flowing in the right direction.
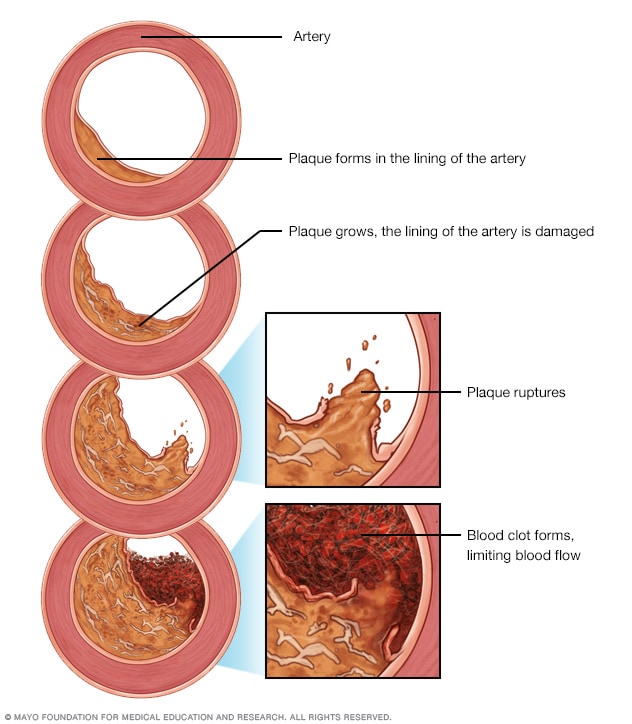
If there's too much cholesterol in the blood, the cholesterol and other substances may form deposits called plaque. Plaque can cause an artery to become narrowed or blocked. If a plaque ruptures, a blood clot can form. Plaque and blood clots can reduce blood flow through an artery.
Risk factors
Risk factors for heart disease include:
- Age. Growing older increases the risk of damaged and narrowed arteries and a weakened or thickened heart muscle.
- Sex. Men are generally at greater risk of heart disease. The risk for women increases after menopause.
- Family history. A family history of heart disease increases the risk of coronary artery disease, especially if a parent developed it at an early age (before age 55 for a male relative, such as your brother or father, and 65 for a female relative, such as your mother or sister).
- Smoking. If you smoke, quit. Substances in tobacco smoke damage the arteries. Heart attacks are more common in smokers than in nonsmokers. If you need help quitting, talk to your health care provider about strategies that can help.
- Unhealthy diet. Diets high in fat, salt, sugar and cholesterol have been linked to heart disease.
- High blood pressure. Uncontrolled high blood pressure can cause the arteries to become hard and thick. These changes interrupt blood flow to the heart and body.
- High cholesterol. Having high cholesterol increases the risk of atherosclerosis. Atherosclerosis has been linked to heart attacks and strokes.
- Diabetes. Diabetes increases the risk of heart disease. Obesity and high blood pressure increase the risk of diabetes and heart disease.
- Obesity. Excess weight typically worsens other heart disease risk factors.
- Lack of exercises. Being inactive (sedentary lifestyle) is associated with many forms of heart disease and some of its risk factors, too.
- Stress. Unrelieved stress may damage the arteries and worsen other risk factors for heart disease.
- Poor dental health. It's important to brush and floss your teeth and gums often. Also get regular dental checkups. Unhealthy teeth and gums makes it easier for germs to enter the bloodstream and travel to the heart. This can cause endocarditis.
Complications
Complications of heart disease include:
- Heart failure. This is one of the most common complications of heart disease. Heart failure occurs when the heart can't pump enough blood to meet the body's needs.
- Heart attack. A heart attack may occur if a blood clot is stuck in a blood vessel that goes to the heart.
- Stroke. The risk factors that lead to heart disease can also lead to an ischemic stroke. This type of stroke happens when the arteries to the brain are narrowed or blocked. Too little blood reaches the brain. A stroke is a medical emergency — brain tissue begins to die within just a few minutes of a stroke.
- Aneurysm. An aneurysm is a bulge in the wall of an artery. If an aneurysm bursts, you may have life-threatening internal bleeding.
- Peripheral artery disease. In this condition, the arms or legs — usually the legs — don't get enough blood. This causes symptoms, most notably leg pain when walking (claudication). Atherosclerosis can lead to peripheral artery disease.
- Sudden cardiac arrest. Sudden cardiac arrest is the sudden loss of heart function, breathing and consciousness. It's usually due to a problem with the heart's electrical system. Sudden cardiac arrest is a medical emergency. If not treated immediately, it results in sudden cardiac death.
Prevention
The same lifestyle changes used to manage heart disease may also help prevent it. Try these heart-healthy tips:
- Don't smoke.
- Eat a diet that's low in salt and saturated fat.
- Exercise at least 30 minutes a day on most days of the week.
- Maintain a healthy weight.
- Reduce and manage stress.
- Control high blood pressure, high cholesterol and diabetes.
- Get good sleep. Adults should aim for 7 to 9 hours daily.
Diagnosis
Your health care provider will examine you and ask about your personal and family medical history.
Many different tests are used to diagnose heart disease. Besides blood tests and a chest X-ray, tests to diagnose heart disease can include:
- Electrocardiogram (ECG or EKG). An ECG is a quick and painless test that records the electrical signals in the heart. It can tell if the heart is beating too fast or too slowly.
- Holter monitoring. A Holter monitor is a portable ECG device that's worn for a day or more to record the heart's activity during daily activities. This test can detect irregular heartbeats that aren't found during a regular ECG exam.
- Echocardiogram. This noninvasive exam uses sound waves to create detailed images of the heart in motion. It shows how blood moves through the heart and heart valves. An echocardiogram can help determine if a valve is narrowed or leaking.
- Exercise tests or stress tests. These tests often involve walking on a treadmill or riding a stationary bike while the heart is monitored. Exercise tests help reveal how the heart responds to physical activity and whether heart disease symptoms occur during exercise. If you can't exercise, you might be given medications.
- Cardiac catheterization. This test can show blockages in the heart arteries. A long, thin flexible tube (catheter) is inserted in a blood vessel, usually in the groin or wrist, and guided to the heart. Dye flows through the catheter to arteries in the heart. The dye helps the arteries show up more clearly on X-ray images taken during the test.
- Heart (cardiac) CT scan. In a cardiac CT scan, you lie on a table inside a doughnut-shaped machine. An X-ray tube inside the machine rotates around your body and collects images of your heart and chest.
- Heart (cardiac) magnetic resonance imaging (MRI) scan. A cardiac MRI uses a magnetic field and computer-generated radio waves to create detailed images of the heart.
Treatment
Heart disease treatment depends on the cause and type of heart damage. Healthy lifestyle habits — such as eating a low-fat, low-salt diet, getting regular exercise and good sleep, and not smoking — are an important part of treatment.
Medications
If lifestyle changes alone don't work, medications may be needed to control heart disease symptoms and to prevent complications. The type of medication used depends on the type of heart disease.
Surgery or other procedures
Some people with heart disease may need a procedure or surgery. The type of procedure or surgery will depend on the type of heart disease and the amount of damage to the heart.
Lifestyle and home remedies
Heart disease can be improved — or even prevented — by making certain lifestyle changes. The following changes are recommended to improve heart health:
- Don't smoke. Smoking is a major risk factor for heart disease, especially atherosclerosis. Quitting is the best way to reduce the risk of heart disease and its complications. If you need help quitting, talk to your provider.
- Eat healthy foods. Eat plenty of fruits, vegetables and whole grains. Limit sugar, salt and saturated fats.
- Control blood pressure. Uncontrolled high blood pressure increases the risk of serious health problems. Get your blood pressure checked at least every two years if you're 18 and older. If you have risk factors for heart disease or are over age 40, you may need more-frequent checks. Ask your health care provider what blood pressure reading is best for you.
- Get a cholesterol test. Ask your provider for a baseline cholesterol test when you're in your 20s and then at least every 4 to 6 years. You may need to start testing earlier if high cholesterol is in your family. You may need more-frequent checks if your test results aren't in a desirable range or you have risk factors for heart disease.
- Manage diabetes. If you have diabetes, tight blood sugar control can help reduce the risk of heart disease.
- Exercise. Physical activity helps you achieve and maintain a healthy weight. Regular exercise helps control diabetes, high cholesterol and high blood pressure — all risk factors for heart disease. With your provider's OK, aim for 30 to 60 minutes of physical activity most days of the week. Talk to your health care provider about the amount and type of exercise that's best for you.
- Maintain a healthy weight. Being overweight increases the risk of heart disease. Talk with your care provider to set realistic goals for body mass index (BMI) and weight.
- Manage stress. Find ways to help reduce emotional stress. Getting more exercise, practicing mindfulness and connecting with others in support groups are some ways to reduce and manage stress. If you have anxiety or depression, talk to your provider about strategies to help.
- Practice good hygiene. Regularly wash your hands and brush and floss your teeth to keep yourself healthy.
- Practice good sleep habits. Poor sleep may increase the risk of heart disease and other chronic conditions. Adults should aim to get 7 to 9 hours of sleep daily. Kids often need more. Go to bed and wake at the same time every day, including on weekends. If you have trouble sleeping, talk to your provider about strategies that might help.
Coping and support
You may feel frustrated, upset or overwhelmed upon learning that you or a loved one has heart disease. Here are some ways to help manage heart disease symptoms and improve quality of life:
- Cardiac rehabilitation. This personalized exercise and education program teaches ways to improve heart health after heart surgery. Cardiac rehabilitation helps add healthy lifestyle changes — such as exercise, a heart-healthy diet and stress management — into your life.
- Support groups. Connecting with friends and family or a support group is a good way to reduce stress. You may find that talking about your concerns with others in similar situations can help.
- Continued medical checkups. Regular appointments with your health care provider can help make sure you're properly managing your heart disease.
Preparing for an appointment
Some types of heart disease will be discovered without an appointment — for example, if a child is born with a serious heart defect, the heart disease will be detected soon after birth. Other times, heart disease may be diagnosed in an emergency situation, such as a heart attack.
If you think you have heart disease or are at risk of heart disease because of family history, see your health care provider. You may be referred to a heart specialist (cardiologist).
Here's some information to help you prepare for your appointment.
What you can do
- Be aware of pre-appointment restrictions. When you make the appointment, ask if there's anything you need to do in advance, such as restrict your diet. You may need to avoid eating or drinking (fast) before a cholesterol test, for example.
- Write down symptoms you're having, including any that seem unrelated to heart disease.
- Write down key personal information — including a family history of heart disease, stroke, high blood pressure or diabetes — and major stresses or recent life changes.
- Make a list of medications, vitamins or supplements you're taking.
- Take someone along, if possible. Someone who goes with you can help you remember information you're given.
- Be prepared to discuss your diet and your smoking and exercise habits. If you don't already follow a diet or exercise routine, talk to your care provider about getting started.
- Write down questions to ask your provider.
For heart disease, some basic questions to ask your health care provider include:
- What is likely causing my symptoms or condition?
- What are other possible causes for my symptoms or condition?
- What tests will I need?
- What's the best treatment?
- Is there a generic alternative to the medicine you're prescribing?
- What are alternatives to the primary approach you're suggesting?
- What foods should I eat or avoid?
- What's an appropriate level of physical activity?
- How often should I be screened for heart disease? For example, how often do I need a cholesterol test?
- I have other health conditions. How do I manage them together?
- Are there restrictions that I need to follow?
- Should I see a specialist?
- Are there brochures or other materials that I can have? What websites do you recommend?
Don't hesitate to ask other questions.
What to expect from your doctor
Your health care provider is likely to ask you questions, such as:
- When did your symptoms begin?
- Do you always have symptoms or do they come and go?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, makes your symptoms worse?
- Do you have a family history of heart disease, diabetes, high blood pressure or other serious illness?
What you can do in the meantime
It's never too early to make healthy lifestyle changes, such as quitting smoking, eating healthy foods and becoming more physically active. A healthy lifestyle is the main protection against heart disease and its complications.
Last Updated Aug 25, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use





