Hypoparathyroidism
Overview
Hypoparathyroidism is an uncommon condition in which the body produces abnormally low levels of parathyroid hormone (PTH). PTH is key to regulating and maintaining a balance of two minerals in the body — calcium and phosphorus.
The low production of PTH in hypoparathyroidism leads to abnormally low calcium levels in the blood and an increase of phosphorus in the blood.
Supplements to bring calcium and phosphorus levels into a normal range treat the condition. Depending on the cause of hypoparathyroidism, you'll likely need to take supplements for life. Sometimes parathyroid hormone replacement is needed if supplements alone are not enough to bring levels into a normal range.
Symptoms
Signs and symptoms of hypoparathyroidism are usually related to low calcium levels in the blood. Signs and symptoms can include:
- Tingling or burning in the fingertips, toes and lips
- Muscle aches or cramps in the legs, feet, stomach or face
- Twitching or spasms of muscles, particularly around the mouth, but also in the hands, arms and throat
- Fatigue or weakness
Other signs and symptoms associated with hypoparathyroidism can include:
- Painful menstrual periods
- Patchy hair loss
- Dry, coarse skin
- Brittle nails
- Depression or anxiety
When to see a doctor
If you have signs or symptoms associated with hypoparathyroidism, see your health care provider for an evaluation. Contact your health care provider immediately if you have a seizure or have difficulty breathing. These can both be complications of hypoparathyroidism.
Causes
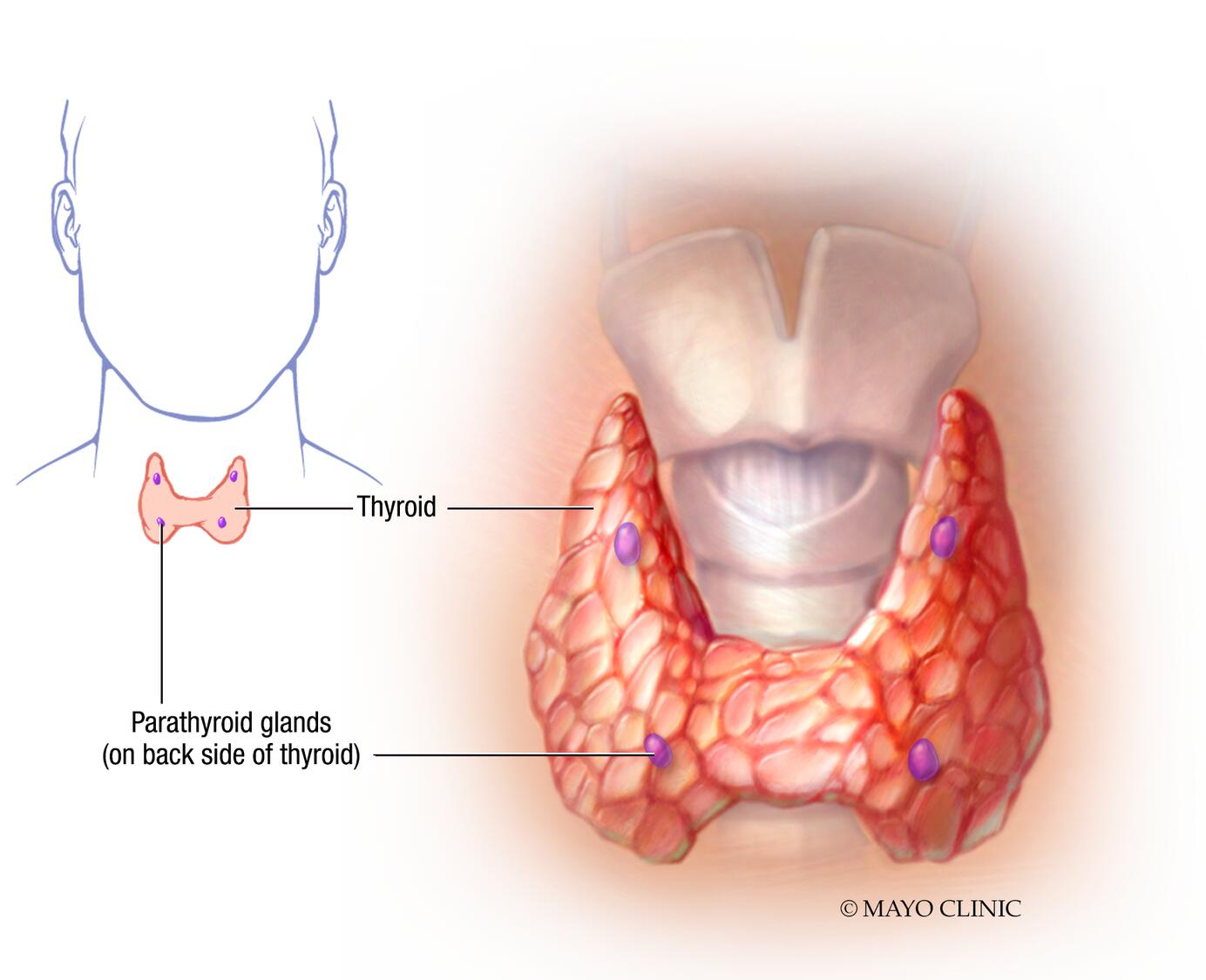
Hypoparathyroidism occurs when the parathyroid glands don't produce enough parathyroid hormone. There are four small parathyroid glands in the neck behind the thyroid gland.
Parathyroid hormone controls the levels of calcium and phosphorus, so too little parathyroid hormone causes abnormal levels of:
- Calcium. This mineral is stored in bones and teeth and makes them hard. Calcium is also needed for muscle function, to help the nerves and brain work properly, and to control heart rhythm and blood pressure.
- Phosphorus. This mineral is found in all cells, but mostly in the bones. Phosphorus is needed to help the body create energy from food. Phosphorus also helps the muscles, nerves, heart and kidneys function.
Causes of hypoparathyroidism can include:
- Neck surgery. This is the most common cause of hypoparathyroidism. It develops after accidental damage to or removal of the parathyroid glands during surgery. Neck surgery may be done to treat conditions of the thyroid gland, or to treat throat or neck cancer.
- Autoimmune disease. In some cases, the immune system attacks parathyroid tissues as if they were foreign bodies. In the process, the parathyroid glands stop producing their hormone.
- Hereditary hypoparathyroidism. This form can result from either being born without parathyroid glands or with glands that don't work properly. Some types of hereditary hypoparathyroidism are associated with deficiencies of other hormone-producing glands.
- Low levels of magnesium in the blood. Low magnesium levels can affect the function of the parathyroid glands. Normal magnesium levels are required for normal production of parathyroid hormone.
- Extensive cancer radiation treatment of the face or neck. Radiation can result in destruction of the parathyroid glands. In rare cases, radioactive iodine treatment for hyperthyroidism may lead to hypoparathyroidism.
Risk factors
Factors that can increase the risk of developing hypoparathyroidism include:
- Recent neck surgery, particularly if the thyroid was involved
- A family history of hypoparathyroidism
- Having certain autoimmune or endocrine conditions, such as Addison's disease — which causes a decrease in the hormones the adrenal glands produce
Complications
Hypoparathyroidism can result in both reversible and irreversible complications.
Reversible complications
Complications due to low calcium levels that may improve with treatment include:
- Cramplike spasms of the hands and fingers that can be prolonged and painful.
- Muscle pain and twitches or spasms of the muscles of the face, throat or arms. When these spasms occur in the throat, they can interfere with breathing, creating a possible emergency.
- Tingling or burning sensations, or a pins and needles feeling, in the lips, tongue, fingers and toes.
- Seizures.
- Problems with kidney function, such as kidney stones and kidney failure.
- Abnormal heart rhythms (heart arrhythmias) and fainting, even heart failure.
Irreversible complications
Accurate diagnosis and treatment might prevent these complications or keep them from getting worse. But once they occur, taking calcium and vitamin D usually doesn't reverse the damage. Irreversible complications include:
- Hardening and changes in the shape of bones, and poor growth
- Delayed mental development in children
- Calcium deposits in the brain, which can cause balance problems, movement disorders and seizures
- Clouded vision due to cataracts
- Teeth that don't form properly, affecting dental enamel and roots, which can happen when hypoparathyroidism occurs at an early age when teeth are developing
Prevention
There are no specific actions to prevent hypoparathyroidism. However, if you're scheduled to have thyroid or neck surgery, talk to your surgeon about the risk of damage to your parathyroid glands during the procedure. Your health care provider may choose to test your calcium, parathyroid hormone and vitamin D levels and have you begin taking supplements if needed before surgery.
Parathyroid autotransplantation may be an option to reduce the chances of postoperative hypoparathyroidism. The surgeon works to preserve parathyroid tissue in the neck during the procedure. However, occasionally the surgeon may need to move parathyroid tissue to another area of the body, such as the arm or the chest muscle. Transplanted parathyroid tissue does not always function.
If you've had surgery or radiation involving your thyroid or neck, watch for signs and symptoms that could indicate hypoparathyroidism, such as a tingling or burning sensation in your fingers, toes or lips, or muscle twitching or cramping. If they occur, your health care provider might recommend prompt treatment with calcium and vitamin D to minimize the effects of the disorder.
Diagnosis
To diagnose hypoparathyroidism, your health care provider will discuss your medical history and do a physical exam, and may suggest blood and urine tests.
Blood tests
These blood test results might suggest hypoparathyroidism:
- A low blood-calcium level
- A low parathyroid hormone level
- A high blood-phosphorus level
A blood-magnesium level may also be done. A low blood-magnesium level may cause a low blood-calcium level.
Urine test
Parathyroid hormone acts on the kidneys to prevent too much calcium from being wasted in the urine. A urine test can tell whether your body is getting rid of too much calcium.
Other tests
Your health care provider may request additional tests, such as other blood tests or a test to check heart rhythm (electrocardiogram, ECG).
Treatment
The goal of treatment is to relieve symptoms and to bring calcium and phosphorus levels in your body back into a standard range.
Treatment usually includes:
- Oral calcium. Oral calcium supplements — as tablets, chews or liquid — can increase calcium levels in your blood. However, at high doses, calcium supplements can cause digestive side effects, such as constipation, in some people.
- Vitamin D. High doses of vitamin D, generally in the form of calcitriol, can help your body absorb calcium and eliminate phosphorus. Calcitriol is a prescription from your health care provider for active vitamin D. This is different from the usual supplements you can get without a prescription.
- Magnesium. If your magnesium level is low and you're experiencing symptoms of hypoparathyroidism, you may need to take a magnesium supplement.
- Thiazide diuretics. If your calcium levels remain low even with treatment, or if the amount of calcium in your urine is very high, thiazide diuretics can help decrease the amount of calcium lost through your urine.
- Parathyroid hormone replacement. The U.S. Food and Drug Administration (FDA) has approved parathyroid hormone (Natpara) for low blood calcium due to hypoparathyroidism. This is a once-daily injection. Because of the potential risk of bone cancer (osteosarcoma), a risk observed in animal studies, this drug is available only through a restricted program. The program limits use to people whose calcium levels can't be controlled with calcium and vitamin D supplements and who understand the risks.
Diet
Your health care provider might recommend that you consult a registered dietitian, who is likely to advise a diet that's:
- Rich in calcium. This includes dairy products, green leafy vegetables, broccoli and foods with added calcium, such as some orange juices and breakfast cereals.
- Low in phosphorus. This means avoiding carbonated soft drinks, which contain phosphorus in the form of phosphoric acid, and limiting processed foods, meats, hard cheeses, nuts and whole grains.
Intravenous infusion
If you need immediate symptom relief, you may need to stay in the hospital so that you can receive calcium by a small tube in a vein in your hand or arm (intravenously). You'll also take oral vitamin D tablets. After you leave the hospital, you'll continue to take calcium and vitamin D tablets.
Monitoring
Your health care provider will regularly check your blood to monitor levels of calcium and phosphorus. At first, these tests will probably be weekly to monthly. Eventually, you'll need blood tests just twice a year. Regular testing allows adjustment of your supplemental calcium dose if your blood-calcium levels rise or fall.
Because hypoparathyroidism is usually a long-lasting disorder, testing and treatment generally is lifelong.
Preparing for your appointment
You'll likely start by seeing your primary care provider. You might then be referred to a specialist in treating hormone disorders (endocrinologist).
Here's some information to help you get ready for your appointment.
What you can do
When you make the appointment, ask if there's anything you need to do in advance, such as fasting for a specific test. Take a family member or friend with you, if possible, to help you remember the information you're given.
Before your appointment, make a list of:
- Your symptoms, including those that seem unrelated to the reason for which you scheduled the appointment, and when they began
- Key personal information, including major stresses or recent life changes and your and your family's medical history
- All medications, vitamins, herbs and other supplements you take, including doses
- Questions to ask your health care provider
Questions to ask may include:
- What is likely causing my symptoms?
- What are other possible causes?
- What tests do I need?
- Is my condition likely temporary or chronic?
- What treatments are available, and which do you recommend?
- What are the alternatives to the primary approach you're suggesting?
- How can I best manage this condition with my other health conditions?
- Should I see a specialist?
- Do I need to change my diet?
- Are there brochures or other printed material I can take? What websites do you recommend?
Don't hesitate to ask other questions during your appointment.
What to expect from your doctor
Your health care provider is likely to ask you questions, including:
- Have you recently had surgery involving your neck?
- Have you received radiation therapy to your head or neck or therapy for treatment of thyroid problems?
- Has anyone in your family had similar symptoms?
- Have your symptoms been continuous or occasional?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
Last Updated May 11, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



