Addison's disease
Overview
Addison's disease, also called adrenal insufficiency, is an uncommon illness that occurs when the body doesn't make enough of certain hormones. In Addison's disease, the adrenal glands make too little cortisol and, often, too little of another hormone, aldosterone.
Addison's disease can affect anyone and can be life-threatening. Treatment involves taking hormones to replace those that are missing.
Symptoms
Addison's disease symptoms usually happen slowly, often over months. The disease can move so slowly that people who have it may ignore the symptoms at first. Then a stress, such as illness or injury, makes symptoms worse.
Symptoms may include:
- Extreme fatigue
- Weight loss and loss of appetite
- Areas of darkened skin
- Low blood pressure, even fainting
- Salt craving
- Low blood sugar, also called hypoglycemia
- Nausea, diarrhea or vomiting
- Abdominal pain
- Muscle and joint pain
- Irritability
- Depression
- Body hair loss or sexual issues in some people
Acute adrenal failure, known as addisonian crisis
Sometimes the symptoms of Addison's disease appear suddenly. Acute adrenal failure can lead to life-threatening shock. Seek emergency treatment for the following:
- Severe weakness
- Confusion
- Pain in the lower back or legs
- Severe abdominal pain, vomiting and diarrhea, leading to dehydration
- Reduced consciousness or delirium
- Low blood pressure
When to see a doctor
See a health care provider if you have common symptoms of Addison's disease, such as:
- Darkened areas of skin
- Extreme loss of body water, also known as dehydration
- Severe fatigue
- Weight loss that doesn't happen on purpose
- Nausea, vomiting or belly pain
- Lightheadedness or fainting
- Salt cravings
- Muscle or joint pains
Causes
Addison's disease is caused by damage to the adrenal glands. The adrenal glands sit just above the kidneys. As part of the endocrine system, they make hormones that affect almost every organ and tissue in the body. Damage to these glands results in too little of the hormone cortisol and, often, the hormone aldosterone.
The adrenal glands are made up of two sections. The interior, called the medulla, makes adrenaline-like hormones. The outer layer, called the cortex, makes a group of hormones called corticosteroids. Corticosteroids include:
- Glucocorticoids. These hormones, including cortisol, affect the body's ability to turn food into energy. They also play a role in the immune system's inflammatory response and help the body respond to stress.
- Mineralocorticoids. These hormones, including aldosterone, balance the body's sodium and potassium to keep blood pressure in a healthy range.
- Androgens. In all people, the adrenal glands make small amounts of these sex hormones. They cause male sexual development. And they affect muscle mass, sex drive, known as libido, and a sense of well-being in all people.
Primary adrenal insufficiency
Sometimes, the outer layer of the adrenal glands, known as the cortex, is damaged. Then it can't make enough hormones, a condition called primary adrenal insufficiency. This is usually the result of an autoimmune disease, in which the body attacks itself. People with Addison's disease are more likely than are other people to have another autoimmune disease as well.
Other causes of adrenal gland failure may include:
- Tuberculosis.
- Other infections of the adrenal glands.
- Spread of cancer to the adrenal glands.
- Bleeding into the adrenal glands.
- Medicines that block the body's ability to make glucocorticoid, such as ketoconazole and etomidate (Amidate). Or medicines that block the action of glucocorticoid in the body, such as mifepristone (Mifeprex, Korlym).
- Treatment for cancer with medicines called checkpoint inhibitors.
Secondary adrenal insufficiency
The pituitary gland makes a hormone called adrenocorticotropic hormone (ACTH). ACTH in turn causes the adrenal cortex to make its hormones. Having pituitary tumors that aren't cancer, inflammation and pituitary surgery can cause the pituitary gland to make too little ACTH.
Too little ACTH can cause the adrenal glands to make too little glucocorticoids and androgens. This is called secondary adrenal insufficiency.
Most symptoms of secondary adrenal insufficiency are similar to those of primary adrenal insufficiency. However, people with secondary adrenal insufficiency don't have darkened skin and are less likely to have severe dehydration or low blood pressure. They're more likely to have low blood sugar.
A temporary cause of secondary adrenal insufficiency occurs when people who take corticosteroids, such as prednisone, to treat conditions such as asthma or arthritis, stop taking the medicine suddenly rather than tapering off.
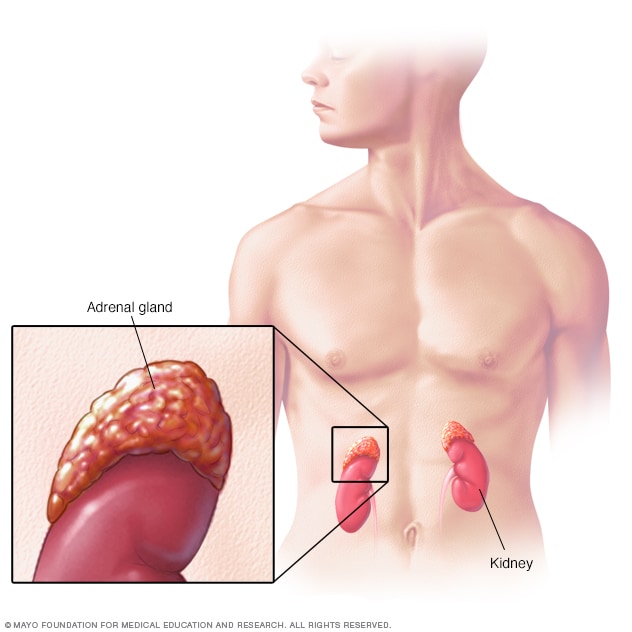
Located on top of each kidney, the adrenal glands make hormones that help regulate metabolism, the immune system, blood pressure and other important functions. Although small, these glands control much of what happens in the body.
Risk factors
Most people who get Addison's disease don't have any factors that put them at higher risk of developing the condition. But the following may raise the risk of developing Addison's disease:
- A history of having a disease or surgery that affects the pituitary gland or the adrenal glands.
- Certain genetic changes that affect the pituitary or adrenal glands. These include gene changes that cause the inherited disease congenital adrenal hyperplasia.
- Other autoimmune endocrine conditions, such as hypothyroidism or type 1 diabetes.
- A traumatic brain injury.
Complications
-
Addisonian crisis. If you have untreated Addison's disease, you may develop an addisonian crisis as a result of stress on the body, such as injury, infection or illness. Typically, the adrenal glands make two or three times the usual amount of cortisol in response to physical stress. With adrenal insufficiency, not being able to increase the amount of cortisol made as a result of stress can lead to an addisonian crisis.
An addisonian crisis is a life-threatening situation that results in low blood pressure, low blood levels of sugar and high blood levels of potassium. It requires immediate medical care.
- Other autoimmune diseases. People with Addison's disease often have related autoimmune diseases.
Prevention
Addison's disease can't be prevented, but there are ways to avoid an addisonian crisis:
- Talk to your health care provider if you always feel tired or weak or are losing weight without trying. Ask about an adrenal shortage.
- If you have been diagnosed with Addison's disease, ask your provider what to do when you're sick. You may need to learn how to increase your dose of corticosteroids.
- If you become very sick, especially if you are vomiting and you can't take your medicine, go to an emergency room.
Some people with Addison's disease worry about serious side effects from hydrocortisone or prednisone. However, people with Addison's disease aren't as likely to get the side effects of high-dose glucocorticoids. That's because the dose prescribed replaces the amount that's missing.
If you take cortisone, be sure to follow up with your provider regularly to make sure your dose is not too high.
Diagnosis
Your health care provider will talk to you about your medical history and your symptoms. You might have some of the following tests:
- Blood test. This test can measure blood levels of sodium, potassium, cortisol and adrenocorticotropic hormone (ACTH). A blood test also can measure antibodies related to autoimmune Addison's disease.
- ACTH stimulation test. ACTH tells the adrenal glands to make cortisol. This test measures the level of cortisol in the blood before and after a shot of human-made ACTH.
- Insulin-induced hypoglycemia test. This test is done to find out if the pituitary gland is causing secondary adrenal insufficiency. The test involves checking blood sugar and cortisol levels after a shot of insulin.
- Imaging tests. A CT scan of the stomach area checks the size of the adrenal glands and looks for other issues. An MRI of the pituitary gland can test for secondary adrenal insufficiency.
Treatment
Medicines are used to treat Addison's disease. Hormone replacement therapy corrects the levels of steroid hormones the body isn't making enough of. Some treatments include oral corticosteroids such as:
- Hydrocortisone (Cortef), prednisone (Rayos) or methylprednisolone (Medrol) to replace cortisol. These hormones are given on a schedule to act like the changes in cortisol levels the body goes through over 24 hours.
- Fludrocortisone acetate to replace aldosterone.
You likely need plenty of salt in your diet. This is especially true during heavy exercise, when the weather is hot or if you have digestive upsets, such as diarrhea.
Your health care provider may increase your medicine for a short time if your body is stressed. Such stress can come from having surgery, an infection or a minor illness. If you're vomiting and can't keep down your medicine, you may need shots of corticosteroids.
Other treatment recommendations include:
- Carry a medical alert card and bracelet at all times. A steroid emergency card and medical alert identification let emergency care providers know what kind of care you need. Also have a written action plan.
- Keep extra medicine handy. It can be dangerous to miss even one day of medicine. So keep a small supply at work and with you when you travel.
- Carry a glucocorticoid injection kit. The kit contains a needle, a syringe and an injectable form of corticosteroids to use in case of emergency.
- Stay in contact with your care provider. Your care provider can monitor your hormone levels. If you have problems with your medicine, your provider might need to change the doses or when you take them.
- Have yearly checkups. At least once a year, see your care provider or a doctor who treats hormone problems. Your provider may recommend yearly screening for autoimmune diseases.
An addisonian crisis is a medical emergency. Treatment typically includes IV:
- Corticosteroids
- Saline solution
- Sugar
Potential future treatments
Researchers are working to develop delayed-release corticosteroids, which act more like the hormones made by the human body. They also are studying the use of pumps placed under the skin that can deliver steroids in more-accurate doses.
Preparing for an appointment
You're likely to start by seeing your primary care provider. However, you might be referred to an endocrinologist, a doctor who treats conditions of the endocrine glands.
Here's information to help you get ready for your appointment.
What you can do
Take a family member or friend with you to help you remember the information you get.
Make a list of:
- Your symptoms and when they began.
- Key personal information, including major stresses or recent life changes.
- All medicines, vitamins or other supplements you take, including doses.
- Questions to ask your provider.
For Addison's disease, questions might include:
- What is likely causing my symptoms or condition?
- What tests do I need?
- Is my condition likely temporary or long-lasting?
- What is the best course of action?
- I have other health conditions. How can I best manage them together?
- Are there restrictions I need to follow?
- Are there brochures or other printed material I can have? What websites do you recommend?
Don't hesitate to ask other questions as well.
What to expect from your doctor
Your provider may ask:
- Do you have symptoms all the time or only sometimes?
- How bad are your symptoms?
- What, if anything, makes your symptoms better?
- What, if anything, makes your symptoms worse?
Last Updated Feb 3, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



