Benign peripheral nerve tumor
Overview
Your peripheral nerves link your brain and spinal cord to other parts of your body. These nerves control your muscles so that you can walk, blink, swallow, pick things up and do other activities.
Several different types of tumors may form on the peripheral nerves. The cause of these tumors is usually unknown. Some have a genetic cause.
Most of these types of tumors are not cancerous (benign). But they can lead to nerve damage and loss of muscle control. That's why it's important to see your health care provider when you have any unusual lump, pain, tingling or numbness, or muscle weakness.
Types
Peripheral nerve tumors affect nerves by growing within them or by pressing against them. Peripheral nerve tumors that grow within nerves are called intraneural tumors. The tumors that press against nerves are called extraneural tumors. Most are benign, meaning that they are not cancerous. Different types of benign peripheral nerve tumors include:
-
Schwannoma. The most common benign peripheral nerve tumor in adults, a schwannoma can occur almost anywhere on the body. These nerve sheath tumors are called schwannomas because they are made up of Schwann cells, which are cells that surround the nerves.
These tumors usually grow slowly. If you develop a schwannoma in an arm or leg, you might notice a mass. But you might have a schwannoma for years before noticing it.
A schwannoma typically comes from a single bundle of nerve fibers, called a fascicle, within the main nerve. Some schwannomas grow and form unusual shapes within the spine or pelvis, such as dumbbell tumors. When a schwannoma grows, more fascicles are at risk when trying to remove the tumor safely.
Schwannomas most commonly occur alone. Occasionally some people have several of them in the arms, legs or body. This is a condition called schwannomatosis.
A rare schwannoma near the brainstem, known as an acoustic neuroma, can cause trouble with balance or hearing. This type of tumor also is known as a vestibular schwannoma. It sometimes occurs in people with a condition called neurofibromatosis 2 (NF2). If acoustic neuromas aren't treated and they continue to grow, they can affect nearby nerves and press on the brainstem.
-
Neurofibroma. This common type of benign nerve tumor tends to form in the center of a nerve. A neurofibroma might arise from several nerve bundles and tends to cause mild symptoms. This tumor most commonly develops in people who have neurofibromatosis 1 (NF1). This is a genetic disorder that causes tumors to grow on nerves.
Symptoms of NF1 include color changes and benign tumors on the skin. Some people who have NF1 develop other conditions. These conditions include bone deformities, such as a curved spine, and an eye nerve tumor called an optic glioma. People with NF1 are at risk of developing a malignant peripheral nerve sheath tumor.
- Perineurioma. This rare benign peripheral nerve tumor arises from perineurial cells, a type of cell that surrounds the peripheral nerve sheath. A perineurioma can form within a nerve, called an intraneural perineurioma. It may also form in soft next to a nerve, called an extraneural perineurioma. An intraneural perineurioma happens most often in children and young adults. It typically causes gradually progressive weakness and loss of feeling in an arm or leg.
- Lipoma. Slow-growing fat cells cause this benign, soft lump that usually appears under the skin on the neck, shoulders, back or arms. A lipoma near a nerve can squeeze it. Usually, though, a lipoma causes no pain or other problems. Your health care provider might want to monitor a lipoma through regular checkups.
- Ganglion cyst. Some ganglion cysts come from an injury, but most have no known cause. They commonly form near joints, such as the wrist, and can cause pain and interfere with everyday activities. Some go away without treatment, but ganglion cysts that press neighboring nerves should be removed.
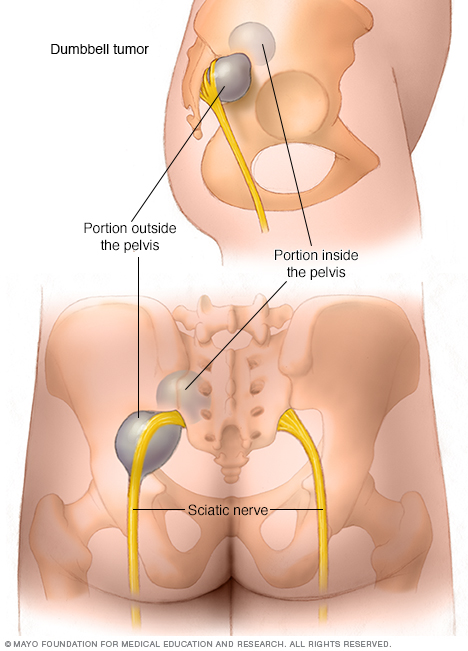
A more complex nerve sheath tumor may assume the shape of a dumbbell. This type of tumor occurs in the spine and lower abdomen and are intertwined with important nerves.
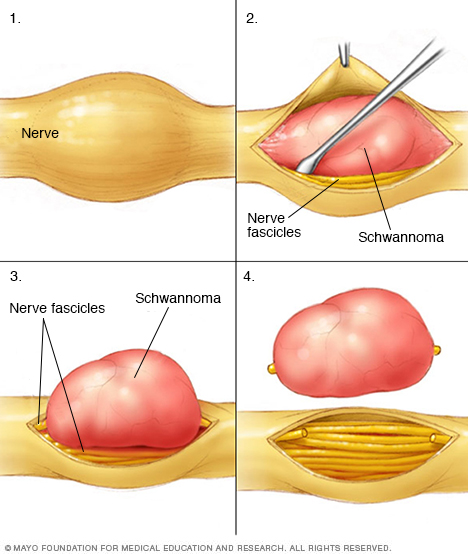
Surgeons carefully remove schwannomas while taking care to preserve nerve fascicles that aren't affected by the tumors. Nerve fascicles are bundles of nerve fibers.
Symptoms
A benign peripheral nerve tumor can cause symptoms if it presses on the nerve in which it is growing or on nearby nerves, blood vessels or tissues.
As the tumor grows, it may be more likely to cause symptoms, but even small tumors can sometimes cause symptoms. Symptoms depend on the location of the tumor and which tissues it affects. Symptoms may include:
- Swelling or a lump under your skin
- Pain, tingling or numbness
- Weakness or loss of function in the affected area
- Dizziness or loss of balance
Causes
The cause of benign peripheral nerve tumors usually isn't known. Some are passed down in families.
The most common type of benign peripheral nerve tumor is a schwannoma. A schwannoma typically starts in a single bundle inside the main nerve, shifting the rest of the nerve.
Another common type is a neurofibroma. A neurofibroma also often forms inside the nerve. Sometimes it grows from several nerve bundles.
Perineuriomas are rare and can grow from inside or outside the nerve. Tumors outside a nerve can cause problems when they press on the nerve. Other benign tumors that form outside nerves are soft lumps of slow-growing fat cells called lipomas and ganglion cysts.
Diagnosis
Your doctor will run tests to find where a peripheral nerve tumor is located and what type of tumor it is.
Tests
You might undergo one or more of the following tests.
- MRI. This is the preferred method for imaging peripheral nerve tumors. This scan uses a magnetic field and radio waves to produce a detailed 3D view of the nerves and surrounding tissue. It can help determine whether you have a tumor and whether the tumor is inside or outside the nerve.
- CT scan. A CT scanner rotates around the body to record a series of images. This test is not as useful as an MRI in diagnosing a peripheral nerve tumor. However, your health care provider might recommend it if you can't have an MRI or if more information regarding the nearby bone is needed.
- Electromyogram (EMG). This test records the electrical activity in a muscle when you try to move it. It is used to help locate the tumor and identify which nerves are involved.
- Nerve conduction study. You're likely to have this test along with your EMG. It measures how quickly your nerves carry electrical signals to your muscles.
- Tumor biopsy. If imaging tests identify a nerve tumor, your care provider might remove and analyze a small sample of cells (biopsy) from your tumor. Depending on the tumor's size and location, you might need local or general anesthesia during the biopsy. The biopsy might be done with a needle with the help of imaging, or it might be done during surgery.
- Nerve biopsy. To help diagnose the type of tumor, your health care provider may take a nerve biopsy. This involves taking a small sample of the tissue and sending it to a lab, where it's studied to look for signs of cancer.
Treatment
Treatment of peripheral nerve tumors involves either surgical removal or observation.
If there's a low likelihood that the tumor may become cancerous and if it isn't causing you problems, you might not need surgery.
Your health care provider might recommend observation if your tumor is in a place that makes removal difficult. Observation includes regular checkups and imaging tests to see if the tumor is growing.
Surgery may be needed if there is a concern that the tumor is cancerous. The tumor also may be surgically removed if it is large or causing pain or other symptoms, such as weakness, numbness or tingling.
Preparing for an appointment
You might be referred to a neurologist or neurosurgeon. A neurologist specializes in disorders of the nervous system. A neurosurgeon is trained in brain and nervous system surgery.
Here's some information to help you get ready for your appointment, and to know what to expect.
What you can do
- Write down when you first noticed the problem and whether it has changed with time.
- Write down your key medical information, including any surgeries.
- Make a list of all your medications, vitamins or supplements.
- Find out if anyone in your family has ever had similar problems.
- Ask a family member or friend to accompany you, to help you remember what you learn during the appointment.
- Write down questions to ask during the appointment.
Questions to ask your doctor
- What's the most likely cause of the problem?
- What kinds of tests do I need?
- What treatments are available?
- I have other health conditions. How can I best manage them together?
In addition to asking questions you've prepared, don't hesitate to ask other questions that come up during your appointment.
What to expect from your doctor
Your health care provider is likely to ask you a number of questions. Being ready to answer them may make time to go over points you want to discuss in-depth. You might be asked:
- Do you have pain? Where is it?
- Do you have any weakness, numbness or tingling?
- Have your symptoms been continuous or occasional?
- What treatments have you tried already for these problems?
Last Updated Oct 19, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use




